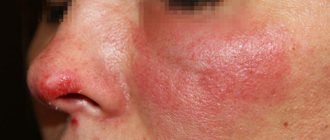
Ringworm is a group of dermatological diseases of viral or fungal origin caused by systemic disorders in the human body. Ointment is one of the most highly effective means for treating the disease, which not only eliminates rashes, burning and peeling of the skin, but also acts directly on the causative agents of lichen.
Types and characteristics of lichen
Lichen is most often found in children; in older people it is diagnosed much less frequently. To treat the disease, pharmacological drugs are used in tablet form that destroy fungi, herpes and other lichen pathogens, as well as medications that eliminate the unpleasant symptoms of the disease. First of all, differential diagnosis is carried out, since the treatment of various types of pathology differs significantly.
| Type of lichen | Signs |
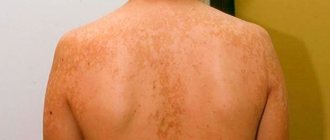
| Shearer | Round spots of a reddish or pink hue, most often affecting the upper body, neck, face and scalp |
| Pink | A brown or bright red spot with a flaky surface that has clear contours and causes itching. Affects the back, abdomen, chest |
| Pityriasis | Small dark brown or beige spots appearing on the skin of the neck, back, and chest. Over time they merge and enlarge, causing itching and flaking |
| girdling | Small spots with bubbles in the center filled with clear liquid. Over time, the bubbles burst, leaving bright red crusts in their place. |
| Red flat | Dark red, brownish, or purple rashes accompanied by intense itching. The rash affects the skin of the arms, legs, abdomen, chest and back |
| Scaly | A chronic disease that affects the skin of the entire body, primarily the areas of large joints. Spots of red or pink color, small |
The dermatologist must take into account what the skin rash looks like and what caused it. You cannot take pills or treat yourself with external remedies. Incorrect treatment can only worsen the situation, cause severe and extensive lesions of the skin and provoke the disease to become chronic.
Why does lichen appear on the skin?
Ringworm has several types depending on the etiology of the disease. But there are several factors that can cause the occurrence of many types of lichen and other dermatological diseases:
- Reduced level of immunity - frequent respiratory diseases, chronic and acute diseases of internal organs, autoimmune diseases.
- Failure to comply with personal hygiene rules, using other people’s personal items: towel, underwear, comb, etc.
- Contact with an infected person or animal;
- Abuse of antibacterial agents / use of household chemicals without gloves - as a result, the barrier functions of the skin are disrupted;
- Visiting public places - sauna, swimming pool, beauty salon, which do not comply with sanitary rules. Be sure to ask the establishment administrator about this;
- Frequent injuries. In case of injuries, wounds should be treated with antiseptic solutions;
- Wearing clothes made of synthetic fabrics.
Reasons for the development of different types of lichen:
- Pityriasis rosea (Zhiber's pityriasis) is often one of the manifestations of allergies; this type is not contagious. May occur after illness or due to severe stress;
- Ringworm is an infectious disease caused by fungi; infection often occurs through interaction with stray animals or an infected person.
- Lichen planus - no specific source of the disease has been identified, appears due to a combination of factors, reduced immunity, long-term use of strong medications and untreated acute diseases.
- Shingles - caused by the herpes virus, against the background of a low level of immunity. The disease is contagious.
- Pityriasis versicolor - the disease has a fungal etiology and develops in the hot season or in a tropical climate.
Many types of lichen have similar symptoms to other skin diseases such as vitiligo, syphilis roseola, herpes, etc., so self-medication is not acceptable.
Remedies for ringworm
Ringworm ointment is one of the most popular and effective medications that can be used to treat skin diseases at home in adults and children. Products for external use have a minimal list of contraindications and very rarely cause side effects.
- Sulfuric
- has a disinfecting, anti-inflammatory and antimicrobial effect, fights redness, peeling and itching, accelerates skin healing. Before applying sulfur ointment, it is advisable to treat the skin with salicylic alcohol. - Terbinafine
- a powerful antifungal agent that cures ringworm on any part of the body. The medication must be applied to the affected areas of the skin twice a day until the symptoms disappear completely. - Exifin
is a pharmacological agent based on terbinafine, used for the treatment and prevention of lichen of fungal origin. Exifin is recommended to be applied to the area of the rash in the morning and evening. The drug has no contraindications and can be used even during pregnancy.
An effective addition to them will be regular treatment of the affected skin with Nitrofungin solution. Throughout the day, the rash area should be treated at least 3-5 times. The course of treatment is 3-6 weeks. Nitrofungin increases the effectiveness of ointments.
Mycoses of smooth skin
Among the widespread fungal diseases today, the most common are mycoses of smooth skin, such as microsporia, trichophytosis, lichen versicolor, mycosis of the feet (hands), and candidiasis. Sources of infection can be sick animals (cats, dogs, mouse-like rodents, cattle, etc.), as well as humans. In recent years, there has been an increase in the number of diseases caused by opportunistic fungi, among which superficial forms of candidiasis are most often recorded. Such a wide prevalence of these mycoses can be explained by the massive use of modern therapeutic agents, the environmental situation and other factors that reduce the body's defenses. One of the reasons for the significant prevalence of mycoses is the weakening of sanitary educational work in recent years. Due to insufficient awareness about the sources and ways of spreading infection, as well as adequate preventive measures, patients turn to the doctor late, and therefore mycoses become chronic, including in children suffering from mycoses of the scalp and smooth skin.
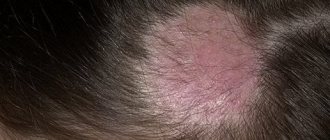
Microsporia is a fungal disease caused by various types of fungi of the genus Microsporum. In Russia, microsporia, which has spread over the last 50 years, is caused by a zoophilic fungus - fluffy microsporum (Microsporum canis), which parasitizes the skin of cats, dogs, and less often other animals. Infection from a sick person is observed in 2% of cases.
Epidemiology . Infection in 80-85% of cases occurs as a result of direct contact with a sick animal or through objects contaminated with the fur of these animals. Infection of children can also occur after playing in the sandbox, since the causative agent of microsporia is highly resistant to environmental factors and can remain viable in infected scales and hair for up to 7-10 years. Children often suffer from microsporia.
Clinic . After 5-7 days from the moment of infection, lesions appear on smooth skin, which can be observed on both open and closed parts of the body (children love to pick up animals and put them in bed with them). The lesions are round or oval in shape, pink or red, with clear boundaries, a raised ridge along the periphery, covered with blisters and thin crusts, with peeling in the center. The lesions are usually small, from 1 to 2 cm in diameter, single or multiple, sometimes merging. In 85-90% of patients, vellus hair is affected.
Treatment . If there are single foci of microsporia on smooth skin without damage to vellus hair, you can limit yourself to only external antifungal agents. The lesions should be lubricated with alcohol tincture of iodine (2-5%) in the morning, and sulfur-salicylic ointment (10% and 3%, respectively) should be rubbed in in the evening. You can rub the following antimycotics 2 times a day: mycozolon, mycoseptin, travogen or 1 time a day in the evening - mifungar cream, mycospor - until the clinical manifestations resolve. In case of multiple lesions of smooth skin and single lesions (up to 3) involving vellus hair, it is recommended to prescribe the antifungal antibiotic griseofulvin at the rate of 22 mg per 1 kg of the child’s body weight, in 3 doses after meals, in combination with exfoliating the stratum corneum of the epidermis in keratolytic lesions means (salicylic acid 3.0, lactic or benzoic acid 3.0, collodion up to 30.0). The lesions are lubricated with one of these products 2 times a day for 3–4 days, then 2% salicylic ointment is applied under compress paper for 24 hours, the detached scales of the stratum corneum of the epidermis are removed with tweezers and vellus hair is epilated. If during a control study carried out using a fluorescent lamp or microscope, affected hair is detected, the procedure is repeated. Detachment of the stratum corneum of the epidermis and manual hair removal of vellus hair can be carried out after using the “sealing” method. The lesions are sealed in a tile-like manner with strips of adhesive plaster for 2-3 days, this causes an aggravation of the process, which, in turn, facilitates hair removal.
The results of treatment for smooth skin microsporia are monitored using a fluorescent lamp or microscopic examination for fungi. The first control study is done after the resolution of clinical manifestations, then 3-4 days before the first negative test, and then after 3 days. The criteria for cure are resolution of the lesions, absence of luminescence and three negative tests on microscopic examination.
During the treatment, bed and underwear are disinfected: boiling in a soap-soda solution (1%) for 15 minutes (10 g of laundry soap and 10 g of caustic soda per 1 liter of water); ironing outerwear, furniture covers, and bedding five times with a hot iron through damp cloth.
Prevention. The main measure to prevent microsporia is compliance with sanitary and hygienic rules (you cannot use other people’s underwear, clothes, etc.; after playing with animals, you must wash your hands).
Trichophytosis is a fungal disease caused by various types of fungi of the genus Trichophyton. Trichophytons can be anthropophilic, parasitic on humans, and zoophilic, whose carriers are animals. Anthropophilic trichophytons include Trichophyton (Tr.) tonsuraus and Tr. violaceum, to zoophiles - Tr. mentagrophytes var gypseum and Tr. verrucosum.
Epidemiology. With superficial trichophytosis, caused by anthropophilic fungi, infection occurs through close contact with a sick person or indirectly through household items. Often children become infected from their mother, grandchildren from grandmothers suffering from a chronic form of the disease. The incubation period lasts up to a week. In zooanthroponotic trichophytosis, the sources of infection are sick animals: cattle, rodents. The highest incidence of this type of trichophytosis is recorded in the fall, which is associated with field work: it is at this time that the likelihood of infection through hay and straw increases. The incubation period ranges from 1–2 weeks to 2 months.
Clinic. On smooth skin with superficial trichophytosis, lesions can appear on any part of the skin - face, neck, chest, forearms. They have clear boundaries of a round or oval shape, with a raised ridge along the periphery of a bright red color; they are larger in size than in microsporia. The lesions are reddish-bluish in color, with peeling, nodules on the surface; in the chronic form, they develop on the skin of the buttocks, knee joints, forearms, less often the back of the hands and other parts of the body; the lesions do not have clear boundaries. Lamellar peeling is observed on the skin of the palms and soles. Vellus hairs are often affected.
With trichophytosis, caused by zoophilic fungi, the disease on the skin can occur in three forms: superficial, infiltrative and suppurative. Lesions are usually located on open areas of the skin. With a superficial form, they are round or oval in shape, with clear boundaries, a raised ridge along the periphery, on which bubbles, crusts, a pink center, and a bright red ridge are visible. The lesions are larger in size than with microsporia. Sometimes they are located around natural openings - eyes, mouth, nose. In the infiltrative form, the lesions rise above the skin level and are accompanied by inflammatory phenomena - infiltration. The suppurative form is characterized by the development of tumor-like formations, bright red in color, covered with purulent crusts due to the addition of a bacterial infection. When the lesion is compressed, pus is released from the hair follicles and pain is noted. The disease is accompanied by a violation of the general condition, sometimes the temperature rises. After the resolution of clinical manifestations, cicatricial atrophy of the skin remains at the site of former lesions. Clinical forms of zooanthroponotic trichophytosis can transform into one another.
Diagnostics. The diagnosis of trichophytosis is established on the basis of the clinic and when the fungus is detected during microscopy of pathological material, and the type of pathogen is determined using cultural examination.
Treatment. Treatment is carried out with antimycotics for external use. The lesions are lubricated with tincture of iodine (2-5%) during the day, and sulfur-salicylic ointment (10% and 3%, respectively) or mycoseptin is rubbed in in the evening. You can carry out monotherapy with ointment or cream (kanison, mifungar, mycozoral, mycospor (bifosin), exoderil, mycozoral, etc. In the infiltrative form, 10% sulfur-tar ointment is prescribed to resolve infiltration 2 times a day. Treatment of the suppurative form of trichophytosis begins with removing crusts from the affected area using bandages with 2% salicylic ointment, which are applied for several hours. After removing the crusts, vellus hair is epilated. Then apply lotions with solutions that have a disinfectant and anti-inflammatory effect (furacilin 1:5000, rivanol 1:1000 , potassium permanganate 1:6000, ichthyol solution (10%), etc.). As a result of this treatment, the hair follicles are freed from pus, inflammatory phenomena are reduced. Next, sulfur-tar ointment (5-10%) is prescribed for resorption of the infiltrate (5-10%) in the form of rubbing or under wax paper.After the infiltrate has resolved, antimycotics are used for external use (see superficial form of trichophytosis).In cases where vellus hair is affected in lesions on smooth skin, the stratum corneum of the epidermis is detached, followed by hair removal. To do this, you can use salicylic collodion (10-15%), milky-salicylic-resorcinol collodion (15%). If there is no effect, griseofulvin is prescribed orally at a daily dose of 18 mg per 1 kg of body weight, in 3 divided doses after meals daily until a negative test for fungi, then every other day. As an alternative method, terbinafine (Lamisil, Exifin) can be prescribed to adults 250 mg (1 tablet) once a day after meals every day, children weighing up to 20 kg - 62.5 mg, from 20 to 40 kg - 125 mg , over 40 kg - 250 mg in combination with antimycotics for external use.
The criteria for cure for trichophytosis are resolution of clinical manifestations and three negative fungal test results at three-day intervals.
Prevention. Prevention of trichophytosis depends on the type of pathogen. With superficial trichophytosis caused by anthropophilic fungi, the main preventive measure is to identify the source of infection, and it can be children suffering from superficial trichophytosis, or adults suffering from a chronic form of the lesion. In recent years, cases of chronic trichophytosis have been observed in middle-aged and older children. For suppurative trichophytosis, preventive measures are carried out jointly by medical workers, epidemiologists and veterinary services.
Mycosis of the smooth skin of the feet (hands). In a number of countries, up to 50% of the population suffers from mycosis of the feet. This disease is more common in adults, but in recent years it has often been observed in children, even infants.
Etiology. The main causative agents of mycosis of the feet are the fungus Trichophyton rubrum (T. rubrum), which is isolated in almost 90% of cases, and T. mentagrophytes var. interdigitale (T. interdigitale). Damage to the interdigital folds, which may be caused by yeast-like fungi, is recorded in 2-5% of cases. The anthropophilic fungus Epidermophyton floccosum is rarely isolated in our country.
Epidemiology. Infection with mycosis of the feet can occur in the family through close contact with a patient or through household items, as well as in a bathhouse, sauna, gym, or when using someone else's shoes and clothes.
Pathogenesis. The penetration of fungi into the skin is facilitated by cracks and abrasions in the interdigital folds caused by sweating or dry skin, abrasion, poor drying after water procedures, narrowness of the interdigital folds, flat feet, etc.
Clinic. Clinical manifestations on the skin depend on the type of pathogen and the general condition of the patient. The T.rubrum fungus can cause damage to the skin of all interdigital folds, soles, palms, dorsum of the feet and hands, legs, thighs, inguinal-femoral, intergluteal folds, under the mammary glands and axillary area, trunk, face, and rarely the scalp. The process may involve vellus and long hair, nail plates of the feet and hands. When the skin of the feet is affected, there are 3 clinical forms: squamous, intertriginous, squamous-hyperkeratotic.
The squamous form is characterized by the presence of peeling on the skin of the interdigital folds, soles, and palms. It can be flour-shaped, ring-shaped, lamellar. In the area of the arches of the feet and palms, an increase in the skin pattern is observed.
The intertriginous form is the most common and is characterized by slight redness and peeling on the lateral contact surfaces of the fingers or maceration, the presence of erosions, superficial or deep cracks in all folds of the feet. This form can transform into dyshidrotic, in which vesicles or blisters form in the area of the arches, along the outer and inner edges of the feet and in the interdigital folds. Superficial blisters open with the formation of erosions, which can merge, resulting in the formation of lesions with clear boundaries and oozing. When a bacterial infection is attached, pustules, lymphadenitis and lymphangitis occur. In the dyshidrotic form of mycosis, secondary allergic rashes are observed on the lateral and palmar surfaces of the fingers, palms, forearms, and shins. Sometimes the disease becomes chronic with an exacerbation in spring and summer.
The squamous-hyperkeratotic form is characterized by the development of foci of hyperkeratosis against the background of peeling. The skin of the soles (palms) becomes reddish-bluish in color, and pityriasis-like peeling is noted in the skin grooves, which extends to the plantar and palmar surfaces of the fingers. Pronounced ring-shaped and lamellar peeling may be detected on the palms and soles. In some patients, it is insignificant due to frequent hand washing.
In children, lesions of smooth skin on the feet are characterized by fine-plate peeling on the inner surface of the terminal phalanges of the toes, usually 3 and 4, or there are superficial, less often deep cracks in the interdigital folds or under the toes, hyperemia and maceration. On the soles, the skin may not be changed or the skin pattern may be enhanced; sometimes ring-shaped peeling is observed. Subjectively, patients are bothered by itching. In children, more often than in adults, exudative forms of lesions occur with the formation of blisters and weeping eczema-like lesions. They appear not only on the feet, but also on the hands.
Rubrophytia of smooth skin of large folds and other areas of the skin is characterized by the development of lesions with clear boundaries, irregular outlines, with an intermittent ridge along the periphery, consisting of merging pink nodules, scales and crusts, with a bluish tint (the color is bluish-pink in the center) . On the extensor surface of the forearms and shins, rashes can be located in the form of open rings. Lesions with nodular and nodular elements are often observed. The disease sometimes occurs as an infiltrative-suppurative trichophytosis (more often in men when localized in the chin area and above the upper lip). Foci of rubrophytosis on smooth skin can resemble psoriasis, lupus erythematosus, eczema and other dermatoses.
The fungus T. interdigitale affects the skin of the 3rd and 4th interdigital folds, the upper third of the sole, the lateral surfaces of the foot and toes, and the arch of the foot. This mushroom has pronounced allergenic properties. With mycosis of the feet caused by T. interdigitale, the same clinical forms of damage are observed as with rubrophytosis, but the disease is often accompanied by more pronounced inflammatory phenomena. In the dyshidrotic, less often intertriginous form, large blisters may appear on the skin of the soles and fingers, along with small blisters; in the case of bacterial flora, with purulent contents. The foot becomes edematous, swollen, and pain appears when walking. The disease is accompanied by an increase in temperature, deterioration of health, development of allergic rashes on the skin of the upper and lower extremities, torso, face, enlargement of the inguinal lymph nodes; the clinical picture is similar to that observed with eczema.
Diagnosis. The diagnosis is established on the basis of clinical manifestations, detection of the fungus by microscopic examination of skin flakes and identification of the type of pathogen by cultural examination.
Treatment. Treatment of mycosis of the smooth skin of the feet and other localizations is carried out with antifungal agents for external use. For squamous and intertriginous forms of lesions on the feet and other areas of the skin, medications are used in the form of a cream, ointment, solution, spray; you can combine a cream or ointment with a solution, alternating their use. Currently, the following medications are used to treat this disease: exifin cream, mycozoral cream, nizoral cream, canizon cream and solution, mycozon cream, mycospor (bifosin) cream, mifungar cream, lamisil cream and spray, mycoterbin cream. These drugs are applied to cleansed and dried skin once a day, the average duration of treatment is no more than 2 weeks. Antimycotics such as travogen, ekalin, batrafen, mycoseptin, mycozolon are used 2 times a day until clinical manifestations resolve, then treatment is continued for another 1-2 weeks, but once a day - to prevent relapse. In nodular and nodular forms of rubrophytosis, after relieving acute inflammatory phenomena using one of these ointments, sulfur-tar ointment (5-10%) is prescribed in order to further resolve the clinical manifestations. For intertriginous and dyshidrotic forms (the presence of only small blisters) of mycosis of the feet, drugs with a combined effect are used, which, along with an antifungal agent, include a corticosteroid, for example mycozolon, travocort, or a corticosteroid and an antibacterial drug - triderm, pimafucort.
In case of acute inflammatory phenomena (wetting, the presence of blisters) and severe itching, treatment is carried out as for eczema: desensitizing agents (intravenous or intramuscular administration of calcium chloride solution (10%), sodium thiosulfate solution (30%), calcium gluconate solution (10%) or calcium pantothenate orally; antihistamines. For external medications, at the first stage of therapy, lotions are used (2% boric acid solution, potassium permanganate solution 1:6000, 0.5% resorcinol solution), 1-2% aqueous solutions of methylene blue or brilliant green, fucorcin. Then they switch to pastes - boron-naphthalan, ichthyol-naphthalan, ACD paste - F3 with naphthalan, if complicated by bacterial flora - lincomycin (2%). At the 2nd stage of treatment after resolution of acute inflammatory phenomena, the above-mentioned antimycotic agents are used.
A drug such as Triderm, which contains, in addition to an antimycotic (clotrimazole 1%), a broad-spectrum antibiotic (gentamicin sulfate 0.1%) and a corticosteroid (betamethasone dipropionate 0), can quickly and effectively eliminate the symptoms of inflammation and itching in the presence of both fungal and bacterial infections. .05%). The presence of Triderm in 2 dosage forms - ointment and cream - makes it possible to use it for different types and at different stages of the pathological process.
If external therapy is ineffective, systemic antimycotics are prescribed: itraconazole in a continuous regimen of 200 mg per day for 7 days, then 100 mg for 1-2 weeks; terbinafine (Lamisil, Exifin) 250 mg once a day every day for 3-4 weeks; fluconazole (150 mg once a week for at least 4 weeks).
Prevention. To prevent foot mycosis, it is necessary to observe, first of all, the rules of personal hygiene in the family, as well as when visiting a bathhouse, sauna, swimming pool, gym, etc.; disinfect shoes (gloves) and linen during the treatment period. After visiting a bathhouse, swimming pool, sauna, to prevent mycosis of the feet, apply Daktarin spray powder to the skin of the interdigital folds and soles.
Tinea versicolor is a fungal disease caused by Malassezia furfur (Pityrosporum orbiculare), a yeast fungus. Lichen versicolor is quite widespread in all countries; young and middle-aged people suffer from it.
Etiology. Malassezia furfur as a saprophyte is found on human skin and, under favorable conditions, causes clinical manifestations.
Pathogenesis. Factors contributing to the development of the disease have not yet been precisely established, however, lichen versicolor is more common in people suffering from excessive sweating, changes in the chemical composition of sweat, diseases of the gastrointestinal tract, endocrine pathology, vegetative-vascular disorders, as well as immune deficiency .
Clinic. The disease is characterized by the presence of small spots on the skin of the chest, neck, back, abdomen, less often the upper and lower extremities, axillary and inguinal-femoral areas, on the head; the spots are initially pink in color and then become light and dark brown; Slight peeling is also observed, sometimes it can be hidden and can only be revealed by scraping. The rashes often merge, forming large areas of damage. After tanning, as a rule, white spots remain as a result of increased flaking. The disease is characterized by a long course with frequent exacerbations.
Diagnosis. The diagnosis is made on the basis of clinical manifestations, when the pathogen is detected in skin flakes during a microscopic examination and in the presence of a characteristic yellow or brown glow under a Wood's fluorescent lamp, as well as a positive iodine test.
Treatment. Currently, there is a sufficient selection of antifungal drugs for topical use that have a pronounced antifungal effect against the causative agent of lichen versicolor. These include imidazole and triazole derivatives, allylamine compounds. During the treatment of the disease, the following is used: exifin cream (applied to cleansed and dried skin in the affected areas 2 times a day for 7-14 days, if necessary, after a 2-week break, the course of treatment can be repeated), nizoral cream, mycozoral ointment, cream and canizon solution, mycozon cream, mifungar cream (prescribed once a day, duration of treatment is 2-3 weeks); lamisil cream and spray; nizoral shampoo (for three days, apply to the affected areas of the skin for 3-5 minutes and wash off in the shower). For common, often recurrent forms of lichen versicolor, systemic antimycotics are more effective: itraconazole (prescribed 100 mg once a day for two weeks, then take a two-week break, repeat the course of treatment if necessary), fluconazole (150 mg once a week within 4-8 weeks). During treatment, it is necessary to disinfect the patient’s clothes, hats, underwear and bed linen by boiling in a 2% soap-soda solution and ironing with a hot iron while wet. Family members of the patient should also be examined.
Prevention. To prevent recurrence of mycosis, it is necessary to use nizoral shampoo. Treatment should be carried out from March to May once a month for 3 days in a row.
Smooth skin candidiasis is a fungal disease caused by yeast-like fungi of the genus Candida.
Etiology. The pathogens are opportunistic fungi that are widely distributed in the environment. They can also be found on the skin and mucous membrane of the mouth, digestive tract, and genitals of a healthy person.
Epidemiology. Infection from the external environment can occur with constant fractional or massive infection with fungi.
Pathogenesis. Both endogenous and exogenous factors can contribute to the occurrence of candidiasis. Endogenous factors include endocrine disorders (usually diabetes mellitus), immune deficiency, severe somatic diseases and a number of others. The development of the disease is possible after the use of a number of modern medications: broad-spectrum antibiotics, immunosuppressive and hormonal drugs. The occurrence of candidiasis in the interdigital folds of the hands is facilitated by frequent contact with water, as this develops maceration of the skin, which is a favorable environment for the introduction of the pathogen from the external environment.
Clinic. On smooth skin, small folds on the hands and feet are more often affected, less often - large ones (inguinal-femoral, axillary, under the mammary glands, intergluteal). Lesions outside the folds are located mainly in patients suffering from diabetes mellitus, severe general diseases, and in infants.
In some patients, the disease begins in small folds of the skin with the formation of small, barely noticeable blisters on the lateral contacting surfaces of hyperemic skin, the process gradually spreads to the area of the fold, then peeling, maceration appears, or immediately shiny eroded surfaces of a deep red color with clear boundaries appear, with peeling of the stratum corneum of the epidermis along the periphery. The 3rd and 4th interdigital folds on one or both hands are most often affected. The disease is accompanied by itching, burning, and sometimes pain. The course is chronic, with frequent relapses.
In large folds, the lesions are dark red in color, shiny, with a moist surface, with a strip of exfoliating stratum corneum of the epidermis, occupying a significant surface, having clear boundaries and irregular outlines. New small erosions appear around large foci. In children, the process of large folds can spread to the skin of the thighs, buttocks, abdomen, and torso. Painful cracks sometimes form deep in the folds.
Candidiasis of smooth skin outside the folds has a similar clinical picture.
Diagnosis. The diagnosis is made on the basis of a typical clinic when a fungus is detected in scrapings from skin flakes during a microscopic examination.
Treatment. Limited and sometimes widespread acute forms of smooth skin lesions, especially those that developed during therapy with antibacterial drugs, as a rule, are easily treated with local antimycotic agents in the form of a solution, cream, ointment and can resolve even without treatment after discontinuation of antibiotics.
For candidiasis of smooth skin of large folds with acute inflammatory phenomena, treatment should begin with the use of an aqueous solution of methylene blue or brilliant green (1-2%) in combination with indifferent powder and continue for 2-3 days, then antifungal drugs are used until clinical resolution manifestations.
Among the antimycotic agents for candidiasis of smooth skin, the following are used: Canison solution and cream, Mycoson cream, Mifungar cream, Candida cream and solution, Triderm ointment and cream, Pimafucort, Pimafucin, Travocort, Travogen, Nizoral cream, Mycozoral ointment, Ekalin.
For common skin processes and in case of ineffectiveness of local therapy, systemic antimycotics are prescribed: fluconazole (Diflucan, Forkan, Mycosist) - adults at a dose of 100-200 mg, children at a dose of 3-5 mg per kg of body weight, itraconazole (100-200 mg), nizoral (adults 200 mg, children weighing up to 30 kg - 100 mg, over 30 kg - 200 mg) once a day daily, as well as the polyene antibiotic natamycin (adults 100 mg 4 times a day, children 50 mg 2–4 times a day). The duration of treatment is 2–4 weeks.
Prevention. Prevention of smooth skin candidiasis in adults and children consists of preventing its development in people suffering from underlying diseases, as well as in people receiving long-term antibacterial, corticosteroid, and immunosuppressive therapy. To prevent the development of candida infection in children hospitalized in somatic departments and receiving broad-spectrum antibiotics, it is necessary to prescribe fluconazole at the rate of 3 mg per kg of body weight once a day, treatment is carried out during the entire main course of therapy. Patients with intestinal candidiasis are prescribed nystatin 2–4 million units per day or natamycin 50 mg for children and 100 mg for adults 2 times a day for 15 days.
Zh.V. Stepanova, Doctor of Medical Sciences, TsNIIKV
Note!
- In recent years, there has been an increase in the number of diseases caused by opportunistic fungi, among which superficial forms of candidiasis are most often recorded.
- Due to insufficient awareness about the sources and ways of spreading infection, as well as adequate preventive measures, patients turn to the doctor late, and therefore mycoses become chronic
- 50% of the population suffers from mycosis of the feet. Adults get sick more often. Recently, there has been an increase in incidence in children, even infants.
- Treatment of mycosis of the smooth skin of the feet and other localizations is carried out with antifungal agents for external use.
- If external therapy is ineffective, systemic antimycotics are prescribed.
Pityriasis rosea
Pityriasis rosea is treated with combination drugs. The most commonly used ointments combine antipruritic, antiallergenic, antimicrobial and anti-inflammatory properties.
- Lorinden A
- has a complex effect, relieves swelling, rashes, itching and burning. The medicine should be applied to the affected areas of the skin 2-3 times a day in a thin, even layer. - Fenistil
is a drug with antihistamine action. Effectively reduces irritation, peeling and rashes. The product is applied up to 3-4 times a day. After applying Fenistil, you need to hide your skin from direct sunlight.
Sinalar
- an effective remedy for pityriasis rosea. It has a complex effect - it fights inflammatory processes, allergic rashes, and destroys pathogenic microorganisms.
Sinalar should be applied to the affected areas of the skin three times a day, lightly rubbing in light circular movements.
The treated area of the body should be covered with a bandage or film. Sinalar should not be used to treat children, as well as women during pregnancy and breastfeeding.
Prevention
To avoid recurrent skin pathology conditions, it is necessary to regularly take preventive measures: lead a healthy lifestyle, eliminate bad habits, include sports, eat a balanced diet and in small portions. In addition, maintain personal hygiene and also remain cautious in public places. It is also necessary to strengthen the immune system and treat other diseases in a timely manner.
Ringworm in humans Pityriasis versicolor Lichen planus Herpes zoster Pink lichen of Zhibera Solar lichen
Medicines for pityriasis versicolor
For the pityriasis form of the disease, antimycotic and keratolytic drugs are used for external use. This type of lichen is also called multi-colored, colored or sunny.
Effective medications for pityriasis versicolor:
- Miconazole
— available in the form of cream and spray, destroys fungal microorganisms. The medicine should be applied to the affected areas of the skin 2 times a day until the rash completely disappears, and then for another 2 weeks to prevent relapse. - Dermazol
- cream and shampoo intended for the treatment of lichen on the head. The medicine is applied to the affected area twice a day for 20-25 days. - Clotrimazole
- This drug can treat pityriasis versicolor on both the skin and scalp. Treatment of deprivation in humans with Clotrimazole ointment has a powerful antifungal effect. Apply to the skin once a day.
A single dose of antifungal tablets for the treatment of solar lichen is prescribed in case of extensive skin lesions, when the rash spreads throughout the body. Among systemic tablets, Fluconazole is most often used - it is taken in a dosage of 150 mg. In the most advanced cases, the medicine is taken for two days - 150 mg per day.
How is pityriasis versicolor transmitted?
Pityriasis versicolor is transmitted through household contact, but this is rare: the disease is not very contagious. The causative agent of pityriasis versicolor, a fungus from the genus Malassezia, is present on the skin of most people, but does not penetrate the epithelium and does not lead to the appearance of a rash. However, under the influence of various factors, yeast transforms into a pathogenic form and begins to destroy skin cells. This process can be triggered by various factors: from excessive sweating to endocrine disorders.
Despite the low contagiousness of this type of lichen, patients are advised to adhere to some recommendations:
- do not share bed linen or towels;
- do not wear other people's clothes;
- do not visit baths, saunas, public swimming pools.
You should also take special care to disinfect the patient’s underwear, clothing and hats: wash at high temperatures (possibly boiling), iron with a hot iron, use steam treatment.
Shingles
Herpes zoster requires an integrated approach that combines systemic medications and the use of antiviral and antiherpetic ointments.
- Acyclovir
- one of the most popular and widespread means for combating herpes virus pathogens. Effectively reduces pain, prevents the appearance of new rashes, accelerates the regeneration of damaged tissues. Acyclovir should be applied to the skin up to 5 times a day for 7-10 days. - Vectavir
- a drug based on penciclovir, blocks further spread of the virus and stimulates skin regeneration. Vectavir must be applied to the skin every 2-3 hours for 5-7 days. - Gerpevir
is a pharmacological agent based on the active component acyclovir. Used in the most complex and severe cases. The course of treatment is 7-9 days, the medicine is applied to the skin 3 times a day.
Additionally, painkillers and non-steroidal anti-inflammatory drugs are prescribed. The doctor may prescribe Ketoralc, Ibuprofen, Naproxen. In the most severe cases, with intense pain, non-steroidal anesthetics are used - Tramadol, Oxycodone.
How to use ichthyol ointment against acne
The ointment effectively helps in the fight against acne. If there are single acne on the face, you need to carefully smear the pimple with ichthyol and cover it with cotton wool. After two hours, you need to remove the ointment.
If there are quite a lot of acne on your face, you can make a mask with ichthyol ointment. You need to spread a thin layer over your entire face, avoiding your eyes and lips. After a couple of hours, remove the mask with a cotton swab, wipe the face with cosmetic milk, and then with diluted salicylic alcohol. You can repeat the procedure a couple of times a week.
It is recommended to make a mask before going to bed, because the ointment has an unpleasant odor.
If there is no result within two months after treatment with the ointment, you should consult a doctor.
Medicines for lichen planus
Lichen planus requires an integrated approach, since this disease can affect not only the skin, but also the mucous membranes of the mouth and genitals.
Rashes are treated with external agents - hormonal creams, gels.
Additionally, drugs to enhance immunity, dietary supplements and multivitamin complexes are used.
- Flucinar
- It is best to start using the medication after the first signs of the disease appear. The medicine is applied in a thin layer twice a day. The course of treatment is 10-14 days. - Fluorocort
- a product for external use that has no age restrictions, it can be used starting from 2 years. Fluorocort should not be used for longer than 14 days. - Prednisolone
is a hormonal ointment that helps with the most advanced and severe forms of lichen planus. Prednisolone is applied to the affected areas of the skin in the morning and evening. The course of treatment is 7-15 days.
Hormonal drugs used for lichen planus include Sinaflan. This glucocorticosteroid quickly relieves signs of the disease - redness, rashes, swelling, itching and peeling. Sinaflan must be applied to inflamed areas of the skin three times a day for 14-15 days.
Can pityriasis versicolor be cured with iodine?
Iodine-containing products are used in the diagnosis of lichen versicolor. Yeast colonies are sensitive to iodine, causing them to absorb it to a much greater extent than surrounding healthy skin. Therefore, if you apply an iodine solution to the epidermis, the affected areas will be much darker.
But many patients believe that iodine is suitable not only for diagnosis, but also for self-treatment of pityriasis. An alcohol solution of iodine is a popular antiseptic that is often used to disinfect the skin. Fungi from the genus Malassezia, which cause tinea versicolor, are sensitive to it and are partially killed upon contact with this substance, but it is impossible to completely destroy them with iodine.
In addition, an alcohol solution of iodine greatly dries already damaged skin, which can lead to various complications of dermatosis.
As a result of self-medication:
- the disease drags on - recovery does not occur, and the rash spreads to new areas of the body;
- the likelihood of relapse increases - after the rash disappears, it appears again when the immune system is weakened and is chronic;
- new symptoms are added to the symptoms of the disease: tightness and dryness of the skin treated with iodine, itching may occur.
Pityriasis versicolor can be cured with antifungal medications prescribed by a dermatologist. Special creams and ointments affect only colonies of the pathogen and do not affect healthy epithelium. Also, many products contain care components that additionally moisturize the skin, accelerate its regeneration and promote the resumption of melanin synthesis.
Therapy for scaly lichen
Lichen squamosus, also called psoriasis, requires a comprehensive approach to treatment. For this disease, systemic medications are used, as well as shampoos and products for external treatment of the skin. The most effective means include:
- Sulfuric
- has an antimicrobial effect, reduces the inflammatory process and the number of psoriatic plaques. The medicine is applied to the skin twice a day, under a sterile bandage until the rash disappears completely. - Salicylic
– fights pathogenic microorganisms and accelerates the regeneration of skin cells. The drug should be applied to the area of the rash three times a day, the course of treatment is 15-20 days. - Naphthalene
- reduces the number of rashes and fights their further appearance. The ointment should be applied to the affected parts of the body for 30 minutes, then blot off the remaining medication with a napkin.
At advanced stages of the disease, hormonal drugs are used - Advantan, Sinaflan, Elokom. They reduce the external signs of lichen, normalize the uncontrolled division of epidermal cells, cleanse the skin and improve its appearance.
What is included in Ichthyol ointment?
The ointment consists of ichthammol and medical petroleum jelly. Ichthammol is a substance made from oil shale resins. It is obtained by gasification and semi-coking. The root of the word is related to the Greek word for fish, which explains the presence of remains of ancient reptiles in the shales.
Ichthyol has been used in medicine since the end of the nineteenth century, thanks to the scientist P. Unn. Initially, a German doctor used it to treat gout, rheumatism and skin diseases. Later it became firmly established in medical practice; an alcohol solution of ichthyol was used in the treatment of migraines. And then tablets with ichthyol appeared, which were taken orally to treat asthenia.
Now there are suppositories with ichthyol and ointment, which are used exclusively externally.
Medicines for lichen in children
Medicines to eliminate lichen in a child must be selected very carefully, because they must not only be highly effective, but also absolutely safe for the child’s health.
Effective ointments for the treatment of pityriasis rosea in children are Tsindol, Flucinar, Lamisil, Zinc, Sulfur and Salicylic ointment.
In most cases, such medications are well tolerated by the child's body and do not cause side effects.
Other drugs for the treatment of lichen in children:
- Clotrimazole
- fights fungal microorganisms, prevents bacterial infections, and cleanses the skin from rashes. - Acyclovir
- used for lichen caused by pathogens of herpes infections. - Mycoseptin
has a pronounced antifungal effect, destroying almost all known types of fungal microorganisms.
Additionally, folk remedy therapy is used with ointments. It is most effective in the initial stages of the disease, with minor rashes. The most effective remedies include decoctions and infusions of celandine, wormwood, and calendula.
Who is prescribed
The following diseases are treated with ichthyol ointment:
- erysipelas;
- eczema;
- burns;
- boils;
- boils;
- neuralgia;
- arthritis;
- haemorrhoids;
- acne.
Suppositories with ichthyol are used for inflammatory diseases in gynecology and urology:
- prostatitis;
- endometritis;
- inflammation of the ovaries;
- salping.
Therapy during pregnancy
Treatment of lichen during pregnancy becomes a serious problem, since most pharmacological drugs are prohibited from being used during pregnancy. Taking into account all the restrictions, pregnant women can use medications based on salicylic acid, sulfur, and tar.
Approved medications include:
- Pimafucin;
- Miconazole;
- Zinc ointment;
- Sulfuric ointment.
Starting from the second trimester, pregnant women can be treated with lichen using the drugs Mycospor, Lamisil, Clotrimazole.
It is strictly forbidden to use hormonal drugs Hydrocortisone, Sinaflan, Advantan, Elokom.
Any glucocorticosteroids during pregnancy can be used only as prescribed by a doctor and under his strict supervision. Folk remedies for the treatment of various forms of lichen can also be used after the permission of the attending physician. They contain medicinal plants that can provoke an allergic reaction and cause unexpected consequences on the part of the fetus.