Who gets scarlet fever most often and when?
Most often, children from 3 to 15 years old suffer from scarlet fever. Newborn children receive immunity from their mother. This immunity protects the baby for about one year. It lasts longer the longer the mother breastfeeds. Children from one to three years old get sick less often simply because they have less contact with peers. When a child begins to attend kindergarten or school, the likelihood of infection increases sharply.
By the age of 15, children come into contact with most varieties of group A streptococcus and develop immunity to them. This means that the risk of developing the disease in adults is small. Scarlet fever is seasonal. Most often, children get it in winter or early spring.
What happens in the body after infection?
Penetration of the scarlet fever pathogen into the body in the vast majority of cases (namely 97%) occurs through the pharynx, less often the “gate of infection” is damaged skin (burns, scratches, wounds - 1.6%), human lungs (1%), sometimes genitals organs (uterine mucosa, so-called postpartum scarlet fever).
Getting on the mucous or wound surface, group A streptococcus - the causative agent of scarlet fever - causes inflammation of the tissue at the site of penetration, followed by death and cell rejection. After the streptococcus penetrates through the lymphatic vessels and blood vessels into the lymph nodes located nearby (in case of infection penetration through the mucous membranes of the upper respiratory tract, the sublingual, submandibular, and cervical groups of lymph nodes are affected).
In the process of its “life activity,” streptococcus produces a toxin that is similar to the autonomic nervous system and the neurovascular system. Causing a chain of pathological changes in the organs and functioning of the patient’s body, the infection determines the main symptoms of scarlet fever in children: increased body temperature, acute inflammation of the tonsils, rash on the skin of the face and body, damage to the cardiovascular system of the body, disturbances in the functioning of the central and autonomic nervous systems.
How is scarlet fever transmitted?
Only people get scarlet fever. Pets cannot be a source of disease. It is transmitted by airborne droplets. For example, when coughing or sneezing. A contact route of transmission is possible - through unwashed hands: by direct touch, through dishes, toys, care items.
With closer contact, the likelihood of disease is much higher. That's why children who attend kindergartens and primary school get sick more often. In this case, the source of infection does not necessarily have to be sick. Especially if this person is an adult. He may simply be a carrier of the infection. This is the reason that many mothers and fathers at my appointment claim that the baby did not meet anyone who was sick, but only communicated with his closest relatives.
Epidemiology
Scarlet fever is currently a rare disease, but it is found everywhere. The source of infection can only be a person.
The disease is called a childhood infection, along with whooping cough, measles, rubella, mumps and chickenpox. These infections are typical mainly for children of preschool and primary school age, since during this period of life they first find themselves in large children's groups, where they can meet a sick or hidden bacteria carrier. In adulthood, the disease is much less common.
From infection to the first symptoms it takes an average of 2 to 7 days4. The peak incidence is observed in the autumn-winter period.
How does scarlet fever occur?
General symptoms:
- acute onset with an increase in temperature to high numbers. Can reach up to 40*C;
- severe weakness, fatigue, malaise, drowsiness, loss of appetite, headache;
- sometimes, as a manifestation of intoxication, nausea and vomiting may occur (one or more times at a high temperature and feeling unwell).
Local symptoms:
- rash. It usually begins 2-3 days after the onset of the disease, but it can also be the very first sign of the disease. Sometimes, with a mild course, a rash may be the only manifestation of scarlet fever. The rash begins from the head and chest. Then it gradually spreads to the whole body. It intensifies in the natural folds of the skin - inguinal, axillary, elbow, knee. Sometimes solid red stripes may form at the folds. Externally, the rash is bright, almost scarlet. If you look closely, you can see tiny bubbles. To the touch it rises somewhat above the surface of the skin, rough. If you press, it turns pale under your finger. Sometimes children are bothered by itching;
- peeling. 3-4 days after the onset of the rash, it begins to gradually turn pale, and the skin in its place dries and peels. At the same time, the scales are very small - 2-3 mm each. Not very noticeable to the eye. Only on the fingers and toes will peeling be pronounced, and the skin will peel off in large thin layers;
- the face has a characteristic appearance - the cheeks are very bright, red. The nasolabial triangle, on the contrary, is very pale;
- changes in the mouth. At the very beginning of the disease, the tongue is covered with a thick white coating. Under it you can see large edematous papillae. After a couple of days, the tongue is cleared of plaque and becomes bright scarlet with clearly defined papillae on it. This is the so-called “raspberry tongue” - a characteristic symptom of scarlet fever. There may be changes in the pharynx characteristic of sore throat. The tonsils become enlarged, reddened and covered with a white or yellowish coating. If you try to pick out the plaque with a spatula, it is easily separated from the tonsil.
Classification and stages of the disease
In Russia, the disease is usually classified according to symptoms, severity and nature of the course (see table below).
Table 1. Classification of scarlet fever
| By typicality of symptoms |
|
| By severity |
|
| According to the nature of the flow |
|
*Atypical forms are relatively rare. With the erased version, the symptoms are very mild, the rash may be completely absent, and the disease quickly regresses within a few days.
Extrapharyngeal variants are characterized by the absence of pharyngitis, typical of scarlet fever. In these cases, the “gateway” of infection becomes, for example, wound and burn surfaces.
Intensified (or aggravated) forms are characterized by a severe course with the development of bleeding, toxic shock and are the most severe variants of the disease.
Features of the disease in adults
In adults, the infection is usually more severe, with severe fever and convulsions. Diagnosis also causes difficulties: usually the doctor does not expect to see scarlet fever in an adult.
Scarlet fever in young children
In children under one year of age, infection is less common. Quite often the disease is complicated by pneumonia, bronchitis, otitis media and other pathologies that increase the scope of treatment.
Scarlet fever in pregnant women
Scarlet fever during pregnancy can cause miscarriages, as well as severe streptococcal postpartum infections in the mother, which are difficult to treat. The main difficulty is due to the fact that during pregnancy the use of antibacterial drugs is limited.
Staging
The infection occurs according to certain patterns. So, they talk about four main periods or stages of the disease:
- Incubation period. The time that passes from infection to the appearance of the first symptoms, that is, the period of active reproduction of bacteria. On average it lasts 2–4 days.
- Initial period. This is the period of time from the appearance of the first symptoms to the appearance of the rash. This period is characterized by the symptoms of intoxication that we have already discussed, a “flaming” pharynx, inflammation of the tonsils and submandibular lymph nodes. This period lasts from several hours to 2 days.
- Rash period. It is characterized by the appearance of a rash in the first 2 days of the disease. While initially bright, the rash fades by 3–4 days of infection. During this period, Filatov’s symptom is observed, later - “crimson” tongue and white dermographism.
- Recovery period. It begins from the 2nd week of the disease, this stage is characterized by peeling of the skin. Specifically large-plate peeling on the palms and soles. During this period, the patient is no longer contagious.
Complications of scarlet fever
Filatov's symptom (left) and a characteristic rash on the body are signs of scarlet fever.
Photo: Estreya at English (Creative Commons Attribution 2.5 Generic license) Complicated course of infection can be caused by toxic, septic and allergic complications. Moreover, the first two types are more often classified as early complications, while allergic ones are mainly regarded as late ones.
The toxic form is characterized by extreme manifestations of intoxication syndrome:
- temperature rise above 40°C;
- repeated vomiting;
- convulsions;
- disturbances of consciousness;
- bright, profuse rash with subcutaneous hemorrhages;
- ECG signs of toxic myocarditis;
- decreased blood pressure;
- (in some cases) death from toxic shock.
The septic form is distinguished by an overly pronounced inflammatory process of a purulent-necrotic nature:
- the tonsils, arches and base of the uvula are inflamed;
- inflammation in the lymph nodes (which can lead to necrosis of the tissues surrounding them);
- bronchitis;
- pneumonia;
- otitis;
- peritonsillar abscess (local accumulation of pus in the tonsil area);
- (in the absence of timely treatment) sepsis and death.
Important! Toxic and septic forms of scarlet fever, as a rule, develop in the absence or incorrectness of treatment. Early competent antibiotic therapy minimizes the risk of such complications.
Complications of the allergic form include:
- myocarditis;
- poststreptococcal glomerulonephritis;
- acute rheumatic fever;
- a number of other pathologies.
The causes of these complications are still the subject of debate. Most often, doctors are inclined to autoimmune disorders that are caused by one of the components of the streptococcal cell wall. Such complications are rarely fatal, but can lead to long-term consequences such as chronic damage to the heart and kidneys.
Diagnosis of scarlet fever
The doctor checks the patient's throat and tongue.
Then, to confirm the diagnosis, blood and an oropharyngeal swab are sent for analysis. Photo: freepik.com When making a diagnosis, doctors are guided by typical symptoms of the disease and a number of clinical and laboratory methods:
- Clinical blood test. The appearance of nonspecific signs of inflammation is characteristic: an increase in the number of leukocytes, an increase in the erythrocyte sedimentation rate (ESR).
- Culture of oropharyngeal swabs. The material collected from the surface of the pharynx is inoculated on special bacteriological media. After cultivation, the properties of the colonies grown on the media are studied and the pathogen is identified.
- Express diagnostic methods. They are based on searching for fragments of a microorganism in material collected from the surface of the pharynx using special reagents.
- A blood test to check for the presence of specific antibodies to streptococcus produced by the body. The study proves the presence of the pathogen in the body.
Instrumental research methods for scarlet fever
Typically, examining symptoms and laboratory tests is more than enough to make a diagnosis. In severe cases of the disease with damage to the heart and kidneys, doctors can resort to instrumental methods for studying them: ECG, ultrasound.
What additional examinations do I need to undergo?
Throat culture or rapid test
In typical cases, the diagnosis is made based on examination and does not require additional research. However, according to international recommendations, before prescribing antibiotics, the child is advised to do a throat culture for flora and sensitivity to antibiotics. Sowing on blood agar, provided proper preparation, is a very sensitive method - up to 95% probability of a correct result. It has only one drawback. You will have to wait 1-2 days for the results. Rapid tests have been developed for faster diagnosis. Their sensitivity is slightly lower. Ranges from 60 to 85%. However, the result can be obtained immediately and without delaying the start of treatment.
In order for a culture or rapid test to show a more accurate value, the child should be properly prepared for the analysis. It will be most effective to do the test in the morning before the baby has eaten, drunk or brushed his teeth. If the test is not done at home, but in a laboratory, it should also not be fed or watered at home. It is allowed to do the test or culture not in the morning, but at least 2 hours must pass from the next meal or drink. If the test is done independently at home, it is important for parents to strictly follow the attached instructions. And take a smear strictly from the surface of the tonsils, it is better from that part of them where the plaque is more abundant. This will increase credibility.
General blood analysis
A general analysis can also be quite informative. It will help the doctor distinguish scarlet fever from a viral infection or an allergic reaction with an unclear clinical picture, and promptly recognize complications.
If complications occur or are suspected, consultations with specialized specialists - ENT, cardiologist, nephrologist - may be necessary; or additional examinations - general urinalysis, biochemical blood test, x-ray, ultrasound, etc.
How to treat scarlet fever?
Scarlet fever is one of the few childhood infectious rashes that can be treated with antibiotics. It must be said that the infection will most likely go away without prescribing an antibiotic, but this greatly increases the risk of complications. Streptococcus is highly sensitive to many types of antibiotics. Penicillins are considered the drugs of choice for children. The doctor must decide which drug is best. It is important to remember that the course of antibiotics for scarlet fever should be at least 10 days.
Despite the fact that the child’s condition usually improves within 2-3 days of taking the medicine. Such a long course is necessary to avoid severe complications of streptococcal infection.
Complications
Although complications from scarlet fever are extremely rare, this disease should never be underestimated. The sooner it is detected, the lower the risk of complications. The main complications after scarlet fever include:
- purulent lymphadenitis
- otitis
- streptococcal arthritis
- myocarditis
- acute glomerulonephritis
- septicemia
- rheumatic fever.
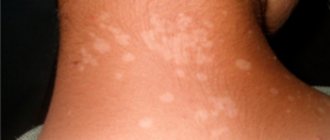
what does a scarlet fever rash look like?
What else can I do to alleviate the condition?
In addition to antibiotics, the child is prescribed local antiseptics and anesthetics - sprays or lozenges. They will help reduce pain and inflammation in the throat.
Sometimes at high temperatures, especially in young children, dehydration can occur. In this case, the baby needs to be given plenty of water. You can also use special pharmaceutical solutions for soldering.
If there is a high temperature and poor health (headache, chills, severe weakness), the doctor may recommend giving the child an antipyretic and analgesic.
Proper care for a sick child is important. For sore throats, warm and sometimes cool drinks and thick drinks (for example, jelly or smoothies) help well. Lollipops are good for soothing sore throats. Not necessarily pharmacy ones, you can give simple candies. It is important to avoid drying out the mucous membranes. Use saline solutions and home humidifiers, ventilate the room. Try to limit physical activity and organize quiet leisure time.
The rash does not require separate treatment. There is no need to spread anything on the skin. Only at the recovery stage, with severe peeling, can wound healing or vitamin ointments be used, after consultation with a doctor.
How can scarlet fever be dangerous?
Provided timely treatment, scarlet fever practically does not cause any complications and goes away completely without a trace.
If antibiotic therapy is not started in a timely manner, acute infectious complications may occur - otitis media, sinusitis, abscesses. The child will complain of a sharp deterioration in health, a repeated increase in temperature to higher numbers. With otitis media, pain in the ear is bothersome. In children, an analogy may be that the child grabs the ear and rips it. Sinusitis causes intense headaches, especially pronounced when bending the head forward or making sudden movements. With a peritonsillar abscess, the pain sharply increases when swallowing, opening the mouth, or turning the head to one side. All these complications require urgent consultation with a doctor and prompt treatment.
Somewhat later, non-purulent complications may develop. Usually 10-14 days after recovery. The most common are reactive arthritis, rheumatism (joint damage), post-streptococcal glomerulonephritis (kidney disease), carditis (heart damage). In order to prevent the development of serious complications, the doctor will advise you to take a general urine and blood test, first a week later, and then 3 weeks after recovery. If there are indications, the doctor may recommend an ECG at the same time.
Treatment methods for scarlet fever
Currently, treatment of scarlet fever, as a rule, does not pose a problem. However, if left without proper treatment, scarlet fever is dangerous due to complications, primarily from the cardiovascular system, kidneys and ENT organs.
After suffering the disease, in most cases, stable lifelong immunity is developed. Recurrence of scarlet fever occurs rarely - only when the immune system is impaired. Immunity is developed specifically to scarlet fever; other streptococcal diseases after scarlet fever are possible.
If you find symptoms of scarlet fever in your child, call a pediatrician at home.
Antibacterial therapy
Streptococcus is highly sensitive to antibiotics, so antibacterial treatment usually leads to rapid improvement and, ultimately, recovery.
Make an appointment Do not self-medicate. Contact our specialists who will correctly diagnose and prescribe treatment.
Rate how useful the material was
thank you for rating
Is it possible to prevent the disease?
There is no specific prevention of streptococcal infection. There is no vaccine for scarlet fever. To prevent infection, you should follow the rules of hygiene:
- washing hands after walking and before eating;
- avoiding close contact with people with tonsillitis or scarlet fever;
- individual dishes. Parents and other family members should not eat from the child's plate; use his spoon; lick your baby's pacifier, bottle, or food;
- Try to isolate a sick family member and provide him with separate hygiene products and utensils. Try to wash and treat them separately (do not put the toothbrush in a common glass; allocate a separate cup, spoon and plate for the entire period of illness; use a separate towel for washing).
Prevention
Since a child with scarlet fever is contagious for 22 days from the onset of the disease, quarantine measures are carried out in kindergarten and school:
- Children who have not had scarlet fever and have been in contact with a sick person are isolated for 7 days (this rule applies to preschool institutions and grades 1-2 of school).
- Children who previously suffered from scarlet fever and recovered children are allowed to visit after 12 days after the elimination of clinical manifestations.
- Admission to a children's institution for those who have recovered from acute respiratory infections, sore throat and other respiratory infections is permitted with a certificate confirming antibacterial treatment.
- Children with sore throat diagnosed within 7 days after the last registration of scarlet fever are also isolated for 22 days from the appearance of the first signs.
- Employees (decreed group) who have not previously been ill and have been in contact with a sick person are allowed to work, and they are subject to 7-day medical observation.
- Current disinfection is carried out with 0.5% chloramine, dishes and linen are boiled. Final disinfection is not practical.
- After illness, employees of children's institutions are transferred to work where they will not be epidemiologically dangerous for 12 days.
Each time after scarlet fever is detected, quarantine is extended for another 7 days.