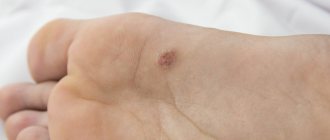
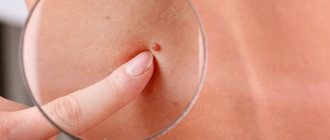
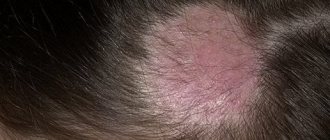
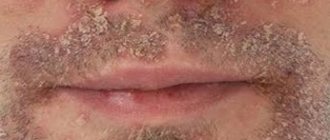
Warts are skin growths in the form of nodules or papillae. This is the most common skin pathology, occurring in more than 90% of the world's population. Warts can appear in any person, at any age, on absolutely all areas of the skin, from the face to the feet. The disease is often contagious, it all depends on the person’s immune system.
COST OF TREATING WARTS IN OUR CLINIC IN ST. PETERSBURG
| Wart removal price | from 500 rub. |
| Dermatologist appointment | 1000 rub. |
| Dermatoscopy | 500 rub. |
| Call free: 8-800-707-1560 *The clinic is licensed to provide these services | |
What causes warts
The content of the article
There is a common belief that touching a frog causes warts to appear. It's a delusion. The causative agent of the disease, which results in the formation of warts, is human papillomavirus infection. According to statistics, this infection causes about 20% of all cancers.
The risk of HPV infection increases significantly:
- when using other people's personal hygiene items and items of common use;
- in public places (swimming pool, bathhouse, etc.), especially when walking there barefoot;
- in case of skin damage;
- with increased sweating of the hands and feet;
- upon contact with an infected person (handshake, sexual contact, etc.);
- when walking in tight, uncomfortable shoes that cause friction on the skin of the foot;
- when using non-sterile instruments (in a beauty salon, etc.).
The infection can remain in the human body for 3 to 6 months without showing itself in any way. Its “activator” and indirect culprit for the appearance of warts is weakened immunity.
Are warts always dangerous?
Most warts are completely harmless and can theoretically disappear in a few weeks or at most a month. In this case, patients are more likely to be concerned about a serious cosmetic defect, which causes psychological discomfort and interferes with leading a full lifestyle.
Warts are often painless unless they are on the soles of the feet or another part of the body that is subject to shock or constant contact. But there are cases of itching and discomfort in the affected area.
But as mentioned above, warts are viral in nature, so you cannot expect that the neoplasm will go away on its own or will not bother you for the rest of your life. Any wart should be shown to a dermatologist, and if he deems it necessary, it should be removed using one of the safe methods.
Dentists' recommendations
Epulis is a gum tumor that poses a great danger to the health of teeth and the entire body. Treatment of the pathology is complex and lengthy, but even with high-quality treatment, the risk of relapse cannot be ruled out.
It is not always possible to prevent the occurrence of epulis on the gums of a child or an adult, but with timely consultation with a specialist, complications, complex treatment, long recovery and aesthetic defects that remain after surgery can be avoided.
The best prevention is to visit the dentist every 6 months. If you are concerned about discomfort and a feeling of rubbing of the mucous membranes or gums, you should immediately consult a dentist, without waiting for a tumor or other pathologies to occur.
How to recognize warts: symptoms and signs
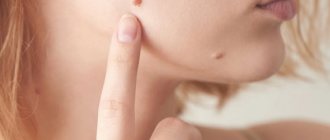
An inexperienced person may confuse warts with other skin growths, for example, moles, calluses, melanomas.
The main differences between warts and moles:
- moles have a dark or black tint, while warts have a light color;
- warts grow tightly together with the skin, moles are separate structures, as if glued to the body;
- moles are soft and smooth to the touch, warts are hard, hard and rough.
It is also easy to distinguish a wart from a callus. When pressing on the growth, painful sensations will occur, and if it peels off, traces of hemorrhages will be visible underneath it. Under the callus is new, tender skin.
You can distinguish a wart from a melanoma by color and shape. This dangerous disease is characterized by heterogeneous red and black shades, proliferation and an uneven contour.
It is not difficult for a dermatologist to make the correct diagnosis using a visual examination. But a good specialist will not be content with just a simple inspection. He will definitely use a special magnifying device - a dermatoscope. If there is a suspicion of a pathogenic process, scraping of the surface layer will be required.
In the case of anogenital warts (located around the anus and on the genitals), consultation with a gynecologist or proctologist is necessary.
Common (simple, vulgar) warts
Common warts are dense, dry growths characterized by an uneven and rough surface to the touch, variable size and rounded shape. They look like a hard, keratinized bubble up to 1 cm in diameter, significantly rising above the surface of the skin.
The surface of common warts is often covered with grooves and projections, which is why the new growth vaguely resembles a cauliflower or raspberry with black dots inside.
This is the most common type of wart, accounting for up to 70% of all such skin neoplasms. Simple warts can appear on the skin at any age, but most often they affect children and young people. This is due to the fact that they have weaker immunity than adults.
Common warts usually appear on the hands (fingers and backs of the hands), knees and elbows, sometimes on the face or feet, and extremely rarely on the mucous membrane of the mouth.
A scattering of small growths may form next to the large “parent” wart. Young neoplasms usually remain flesh-colored; over time, they acquire a dirty gray or grayish-brown tint, less often yellow or pinkish. This is due to their uneven porous surface, which accumulates dirt.
Vulgar warts usually do not cause concern: they do not cause unpleasant symptoms, do not hurt or itch. However, they may cause pain if they are in areas subject to impacts or in contact with clothing. The growths may heal on their own over time, especially if they occur in childhood.
Reasons for education
After conducting numerous studies, scientists have not been able to determine an exhaustive list of factors that provoke the development of pathology. However, some conditions and phenomena still occur most often when diagnosing this disease. For example, this is possible with a hereditary predisposition to fibroids on the gums (shown in the photo below), tongue, inside the cheeks and other areas of the mucous membranes. In this case, the disease develops in childhood in young patients from 1 to 10 years.
Often, in the presence of this diagnosis, a history of regular traumatic exposure is established. There may be constant biting of a certain area of soft tissue. They can also be injured by sharp edges of crowns, orthodontic structures, dentures, especially poorly fixed ones, and hard food.
Taking certain medications can also be a provoking factor. Some medications can cause the appearance of benign lumps in representatives of different age categories, not only in children and adolescents. Drugs that may cause fibromatosis after use:
- Cyclosporine. It is indicated to prevent organ rejection during transplantation.
- Valproate, used by epileptics.
- Verapamil and other calcium channel blockers.
- Estrogens of synthetic origin in oral contraceptives or other hormonal pills.
The culprits in the development of the disease may be inflammatory processes in the oral cavity. These include stomatitis, glossitis, periodontal disease, gingivitis, etc.
It is impossible to exclude a hereditary factor, but the risk of formations can be significantly reduced if you follow simple preventive rules:
- do not forget about hygiene;
- Carry out regular professional cleaning to remove thick plaque and tartar;
- protect soft tissues from traumatic effects (solid food, biting), and also avoid sudden temperature changes;
- treat dental diseases in a timely manner;
- consult with doctors before starting to take medications and avoid self-medication;
- visit the dentist for preventive maintenance at least once every six months.
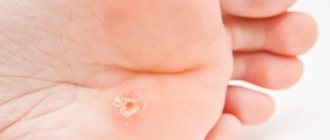
Plantar (spike) warts
Plantar warts are a type of vulgar wart. The manifestation of the disease is most often observed in children and at the age of 20-30 years. Of all skin warts, plantar warts occur in 30%.
Warts on the soles appear as hard, round lumps with papillae in the middle. Inside the wart, characteristic black dots are visible - many small thrombosed capillaries. Along the edges there is a small roll of keratinized skin. The visible part, rising above the surface of the skin by only 1-2 mm, can reach 2 cm in diameter and is only a quarter of the total size of the plantar wart, which mainly forms in the deep layers of the epithelium (skin).
Externally, the spine resembles a callus. A plantar wart can be differentiated (distinguished) from a callus by the visible interruption of the skin pattern in accordance with the wart.
This type of neoplasm usually affects the feet (sole, sides and toes), and less commonly the palms. They appear on the skin as small whitish, pinpoint skin lesions, sometimes itchy. Over time, their surface becomes rougher and changes color - from yellow to dark brown.
Plantar warts themselves do not pose a threat to health, but when walking they cause a person significant discomfort, cause pain, which often intensifies, and can even bleed. This is due to the location of the tumor and the specifics of its growth. Since the spine grows inward, the weight of the body when walking compresses the pain receptors.
The incubation period of the disease ranges from several days to several years. The infection enters the body and goes into waiting mode for a favorable environment to activate. Plantar warts regress without treatment in 50% of cases. But this process lasts from 8 months to one and a half years.
Without treatment, plantar warts will enlarge and multiply, even to the point of producing large clusters of tumors. This can even lead to temporary loss of a person's ability to work due to unbearable pain that prevents walking.
Based on the characteristics of the lesion and its location, plantar warts are divided into 3 types:
- simple;
- periungual;
- mosaic.
Why does a lump appear on the gum?
The accumulation of conditionally pathogenic and pathogenic microflora due to improper oral care leads to inflammation of the mucous membrane. Other reasons why a ball appears on the gum include:
- chemical, thermal or mechanical trauma to the periodontium;
- carious formations and their complications: periodontitis, pulpitis;
- inflammation of the wisdom tooth;
- eruption of molars;
- jawbone overgrowth;
- weak immune system;
- infectious pathologies of the oral cavity: herpes, candidiasis, stomatitis.
A lump in the mouth also occurs under other conditions: epulis, exostosis, fibroma, focal fibromatosis, malignancy, cyst and flux. The main thing is to promptly establish the causes of the pathology and begin treatment.
Periungual plantar warts
Periungual warts are small, rough formations with cracks on the surface, located on the hands and feet of a person, namely near the nail plate or deep under it. Externally they resemble cauliflower heads.
They can be flat, pointed or hemispherical. As a rule, periungual warts are gray, but they can also be flesh-colored. They are not too dense, like simple plantar ones, but have a fairly deep root.
This disease mainly affects children and young people. The main factor in contracting the infection is skin microtraumas around the nail. At particular risk are those who bite their nails and pet stray animals, as well as people who carelessly remove cuticles, use undisinfected tools, and work in water without gloves.
This type of neoplasm does not pose a threat to human health; it is mainly only a cosmetic defect. Periungual plantar warts do not cause discomfort or pain when pressed. However, a wart under the nail is not so harmless - over time, the neoplasm provokes depletion of the nail plate and its further destruction.
In addition, various bacteria and viruses enter through cracks on the surface of the growths, which easily form due to frequent hand work, causing re-infection. Also, as warts grow, the cracks can cause pain. The cuticle is often lost and a tendency to become inflamed (paronychia) develops.
Removal of the tumor is necessary to stop the proliferation of growths, which easily spread to healthy fingers. Localization of the wart under the nail plate makes treatment and removal very difficult. When it appears in childhood or adolescence, it can go away on its own.
Treatment of neoplasms in the oral cavity
A lump under the jaw or on the gum can be detected upon examination. For an accurate diagnosis, a biopsy or x-ray is prescribed. Treatment is selected taking into account the cause of the formation of a bubble in the oral cavity. It will be necessary to stop the further spread of infection and eliminate discomfort.
The doctor will determine how to remove the lump after a complete diagnosis, but the main measures include:
- fistula - pus is removed by rinsing with a disinfectant solution;
- epulis - surgical intervention (removal using diathermocoagulation, cryodestruction or a scalpel);
- periodontitis - removing fillings, cleaning canals, removing pus, rinsing with herbal decoctions and soda solution;
- periostitis - placement of special drugs under a temporary filling (if there is no result, the tooth will have to be removed);
- gingivitis - cleaning of periodontal tubules, antiseptic and antibacterial therapy, removal of lumps.
When a formation appears on the gum, you can rinse your mouth with vodka, diluted alcohol or juice from fresh Kalanchoe leaves.
Timely diagnosis allows you to prevent further spread of infection and save teeth.
Only an experienced dentist will help you get rid of a lump in your mouth, minimizing the risk of developing serious complications. At the first signs of pathology, you should immediately consult a doctor. The doctor's consultation
Mosaic plantar warts
Mosaic warts are a special type of neoplasm. They are plaques, so-called clusters, formed as a result of the fusion of many small plantar warts tightly pressed together. The arrangement of the plaques resembles a mosaic (hence their name).
This formation is usually observed in a small and localized area. It can reach a diameter of about 6-7 cm. In the early stages of development, mosaic warts look like small black punctures. As they develop, they take on the appearance of a white, yellowish or light brown cauliflower, with dark spots in the middle. These spots are formed due to thrombosis of blood vessels.
This type of wart is quite rare. They usually affect the hands or soles of the feet, and are especially common under the toes. Unlike simple plantar warts, mosaic warts cause little or no pain when walking because they are flatter and more superficial.
Mosaic warts are highly contagious. They are difficult to treat due to the multiplicity of foci of viral infection. The success of treatment is facilitated by its timely initiation. As a rule, mosaic growths are prone to recurrence even after surgical removal.
What reasons can lead to its appearance?
The main cause of epulis on the gums is considered to be constant mechanical impact (rubbing) of soft tissues.
Injury to one area can cause gum swelling:
- poorly installed seal;
- uneven edges of the opposite tooth, which is destroyed or chipped;
- tartar;
- poor quality or incorrectly installed prosthesis;
- agonist tooth for malocclusion;
- adjacent teeth when teeth “pile up.”
Supragingival tissue occurs and, as a consequence, injury to epithelial tissue as a result of a burn, bruise or constant ingestion of irritating foods. In pregnant women, tumors occur due to hormonal imbalances. Epulis on a child’s gums can form due to general causes or disturbances in the eruption of permanent teeth.
Flat (juvenile) warts
Flat warts are a fairly common type of tumor and the least problematic. They present as small lenticular lesions (several mm in diameter) or smooth papular lesions. They can grow either singly, which is quite rare, or in large numbers, close to each other.
There are several stages of the disease:
- mild – one or several painless warts;
- medium – from 10 to 100 painless growths;
- severe – more than 100 neoplasms.
If they are localized in places that experience excess pressure (friction from clothing, shoes, etc.), they cause pain.
Flat warts are easily identified and have a white, brown, yellowish or pink hue, similar to the color of meat. They are about the size of a pinhead and, compared to other types of warts, are smoother and flatter. In fact, at the point where a flat wart develops, the skin rises slightly (to a height of about 5mm), forming a sort of raised circular area.
The growths typically appear on the face, knees, elbows, back, legs, and arms (especially the fingers). People of absolutely any age become victims of this disease. But most often it affects children and adolescents (20% of schoolchildren have it), hence the second name for warts - juvenile.
In a close group of schoolchildren, 80% show resistance (resistance) to the virus. In adults, irritation and inflammation after shaving contribute to the proliferation of tumors.
The incubation period of infection can last up to 8 months. Mostly the disease is only a cosmetic defect. Juvenile warts are painless unless caused by mechanical pressure or injury and can sometimes cause itching, but are extremely contagious.
The virus is practically not transmitted through shared objects; the main route of infection is skin contact. Flat warts multiply so easily that it is enough to touch a healthy part of the body to cause the birth of a new formation.
The peculiarity of this type of wart is that in most cases no treatment is required: they can disappear as suddenly as they appeared, especially in children. In adults, the disease must be treated, and the virus is very resistant to drug treatment.
Anogenital warts (condylomas)
Among sexually transmitted diseases, anogenital warts are especially common. They are flat and elongated neoplasms or elastic elastic growths in the form of cauliflower or cockscomb. Such warts reach 1-1.5 cm and are gray, pink or flesh-colored.
Typically, this type of neoplasm is transmitted sexually: during vaginal/anal sex or even simply through contact with intimate areas without penetration. After oral sex, warts can appear on the mucous membranes of the mouth, throat, vocal cords or trachea. Such growths are called oral, or acute, condylomas. In rare cases, infection occurs through household contact or from mother to newborn.
Based on their appearance and structure, there are several types of genital warts:
- Pointed - loose polyps of pink, flesh-colored or red color, on a stalk or a wide base, reminiscent of cauliflower. They can occur either individually or in the form of multiple clusters. Genital warts are prone to rapid reproduction;
- Papillary - round, smooth growths without a stalk, rising above the surface of the skin by several millimeters;
- Keratotic - very dense, thickened formations that protrude significantly above the skin. Typically affects the female labia majora;
- Giant (Buschke-Levenshtein condylomas) are a rare type of wart. They are prone to rapid growth, accompanied by destruction of surrounding tissues. In extremely rare cases, giant condyloma degenerates into a malignant form;
- Flat - formed both singly and in the form of multiple clusters. There are practically no symptoms, sometimes itching and discharge may occur. The affected area of flat growths is the vaginal mucosa and cervix in women.
The appearance of anogenital warts and the deterioration of their condition are often accompanied by other sexually transmitted diseases (ureaplasmosis, trichomoniasis, chlamydia, etc.). It is impossible to protect yourself or your partner from infection using a condom, since in this case it is ineffective. It is necessary to completely abandon intimate relationships until complete recovery.
Anogenital warts occur equally often in people of both sexes who are sexually active (usually from 20 to 25 years). The incubation period for this disease varies from three weeks to nine months, with an average of about three months.
In men, condylomas are most often found on the foreskin, scrotum, inside the urethra and on the penis. They can be localized around the anus and rectum, especially in homosexual men. In women, warts appear mainly at the level of the vulva, vaginal wall, cervix and perineum; The urethra and anal area may also be affected.
Genital warts are more common in immunocompromised patients. The rate of growth varies, but pregnancy, immunosuppression (suppression of the immune system), discharge from the urethra, vagina or rectum, accumulation of smegma, or skin maceration (the natural process of swelling of the epidermis (layer of skin) with prolonged contact with liquid) can accelerate the growth and spread of warts.
Characteristic symptoms of the disease:
- severe itching at the location of the growth;
- painful and uncomfortable sensations;
- burning;
- pain during and after sexual intercourse;
- foreign body sensation;
- problems with defecation when the wart is located in the anus;
- bleeding when condyloma is damaged.
In most cases, anogenital warts are benign, but they can degenerate into carcinoma. For this reason, in order to prevent cancer, condylomas, regardless of their position, shape and size, are always removed.
Anogenital warts are usually diagnosed clinically. Their morphology distinguishes them from typical lateral condylomas of secondary syphilis, but in any case, serological tests for syphilis are necessary in the initial phase and after 3 months. A biopsy is required to rule out carcinoma and is mandatory in cases of bleeding, ulceration or persistent warts.
Endocervical and anal warts can only be visualized by colposcopy and anoscopy. Application of a solution of 3-5% acetic acid for a few minutes before colposcopic examination causes the growth to change color to white, improving visualization and detection of small warts.
Recurrence of anogenital warts is promoted by:
- promiscuity;
- lack of personal hygiene;
- installation of an intrauterine device, termination of pregnancy using surgical traumatic methods or other medical procedures.
This type of wart is dangerous due to a number of complications:
- Lack of careful intimate hygiene or irritation of growths due to constant friction against underwear leads to ulceration of growths by secretion of purulent discharge with an unpleasant odor;
- In the absence of timely treatment, genital warts are prone to suppuration;
- Lack of therapy leads to the formation of a large number of warts. In particularly advanced cases, not even a small area of healthy skin remains;
- In the presence of anogenital warts, a strong decrease in immunity is observed, which is associated with a person’s susceptibility to any infectious disease. If the patient already has a chronic inflammatory disease (in particular, of the pelvic organs), it will necessarily get worse;
- Threat of degeneration into a malignant form.
Treatment of oral fibroids
Surgery remains the most effective and most common therapeutic method. The seal is excised using a laser or radio waves. This procedure lasts about half an hour. If the tumor is very large, after its removal the wound is covered with a flap, which is formed by the doctor from the surrounding tissue.
When pathology is caused by taking certain medications, they should be completely eliminated and replaced with alternatives with similar properties. After discontinuation of drugs in such cases, the appearance of the mucous membranes is often restored without outside help, and the likelihood of relapse approaches zero. However, this does not apply to situations where the disease is advanced.
Surgery can also be avoided in case of traumatic effects of orthopedic structures. For example, when a crown, filling, or prosthesis puts pressure on the tissue. Elimination of the provoking factor often leads to a decrease or complete disappearance of a benign formation. Most likely, it will be necessary to dismantle the old structures and replace them with new ones.
On the Internet you can find stories of healing using home remedies. It is worth remembering that the disease cannot be treated with the help of folk recipes. Herbal decoctions and infusions, and other compositions are used only as an auxiliary element of complex therapy.
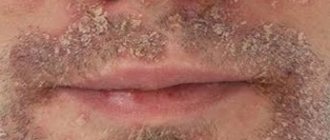
Filiform (acrochord) warts
Filiform warts, also known as facial warts, are the most unusual type of these growths. They are thin, long, racem-like shoots that are usually found on the eyelids and surrounding areas, on the neck, near the lips and nose, and less commonly on the legs, in the groin folds, under the mammary glands and in the armpits.
The typical color of acrochords is flesh-colored, which is why people do not immediately notice them. Sometimes they may turn yellow, brown or pink. Usually they reach a length of 5 to 10 mm, extremely rarely - several centimeters. Depending on the severity of the virus, acrochords form singly or in multiple clusters. This distinctive type of filamentous wart is usually diagnosed visually.
Filiform warts form when a strain of the human papillomavirus causes the top layer of skin to grow too quickly. At the inception stage, the growth looks like a yellowish bump. As it grows, it stretches out, transforming into an elongated formation on a stalk. To the touch, the wart has an elastic and dense structure.
People of absolutely any age can become a “target”, but often elderly patients suffer from this disease. According to statistics, about 50% of the world's population over 50 years of age have facial warts.
Infection with the virus often occurs through cracks and abrasions on the face, so people with dry skin are at high risk. Also, the appearance, growth and spread of facial warts is facilitated by various hormonal changes (pregnancy, obesity, menopause, ovarian dysfunction, diabetes, etc.).
Although highly contagious (infectious) and unattractive in appearance, this type of wart is benign, painless, and often responds well to treatment.
When they appear in sensitive areas, such as skin folds, or areas often subject to pressure and injury, some symptoms may occur:
- itching;
- bleeding;
- soreness;
- irritation.
This type of wart almost never develops into a malignant form. However, if the acrochord is injured, there is a high risk of developing an inflammatory process. Unlike many other similar neoplasms, the filamentous type does not disappear on its own. When a wart falls off, a new one grows in its place. Sometimes there is keratinization of the growth and its transformation into a cutaneous horn.
Facial papillomas are contagious and can be spread by sharing towels or facial cosmetics. Touching the acrochords puts a person at risk of spreading them to other parts of the body. Warts will increase in size and number if they are not removed.
Their location and ugly appearance make facial growths a cause of emotional stress and embarrassment for many people, sometimes affecting their self-esteem and self-confidence.
Symptoms
The tumor grows and develops quite slowly, so for a long time the patient may not even be aware of its presence in the mouth. Fibroma of the oral mucosa looks like a hemispherical growth rising above the plane, covered with pinkish tissue. If you press it, pain or other discomfort does not appear. The surface is smooth, there are no irregularities or roughness on it.
The appearance of ulcers with such a diagnosis is very rare. In such cases, an infection is usually associated with the subsequent development of the inflammatory process. Swelling, redness, erosion occur, and pain is felt. The pain persists even if you do not touch the pathological area.
If you do not injure the formation, it may not change its size for quite a long time and remain in a stable state. If it is exposed to constant traumatic effects, there is a high risk of malignant degeneration, which is dangerous to the life and health of the patient.
Senile (age-related keratomas, seborrheic keratoses) warts
Senile warts are one of the most common skin lesions that appear in old age as a general sign of skin aging. Despite their name, they are not caused by the human papillomavirus.
Seborrheic keratoses are extremely common. According to statistics, more than 90% of the population over the age of 60 have one or more of them. They are equally common in both men and women. It is not uncommon for the disease to affect people aged 30-40 years, as well as young people under 20 years of age.
Keratomas and keratoses can appear on any part of the body, including the scalp, face and genitals. The exception is the palms, soles of the feet and mucous membranes. It is rare for a person to develop only one growth. Over time, age-related keratomas become more and more numerous. Many people inherit a tendency to develop a very large number of these tumors. Some of them may have hundreds of wart-like growths scattered throughout their body.
In the early stages, aging warts appear as slightly raised light brown spots or papules. They can remain very flat and resemble freckles in appearance, or they can gradually thicken and develop a rough, warty surface, like a tumor on the skin. In most cases, they darken slowly and may eventually turn black.
These color changes are harmless. Many senile warts remain pinkish in color. Typical of these are small keratin plugs that can be seen on the surface of the wart.
Keratoses are usually round or oval in shape. Some seborrheic warts are irregular in shape. Their size can vary from one to several centimeters in diameter.
The cause of age-related keratomas is unknown. They are generally considered to be degenerative in nature and appear in large numbers as the skin ages. It is assumed that ultraviolet radiation increases the likelihood of their development.
There are five traditional forms of age-related warts:
- Spotted, or popularly “death freckles” . They form in numerous clusters on the hands and face. Such growths are round with an uneven contour and a smooth or slightly rough surface. It has several color options: light brown, brown-brown or pinkish-yellow;
- Papular or nodular . Larger growths tend to grow. Their typical color is gray or yellow. The surface of the wart is covered with horny layers;
- Classic keratoma . It is a collection of plaques tightly connected to each other. It is characterized by a jagged outline and a copper or pinkish color. As it grows, the middle part of the wart sinks;
- Cutaneous horn. It is a modification of keratoma. It is expressed as a cluster of dense keratinized dark brown plaques up to 1.5 cm.
Adverse reactions to certain medications and many chemotherapy drugs can contribute to the formation of irritated seborrheic keratoses—inflamed, red, crusty lesions. This leads to the development of eczematous dermatitis around the growth. Dermatitis can also cause new seborrheic keratoses to appear.
Age-related keratomas are always benign. This means that they do not spread and do not degenerate into a malignant form. The main problem is a cosmetic defect, especially if they develop on the face.
There are rare cases of skin cancer called melanoma that develops in a seborrheic wart. It is unknown whether this is just a coincidence or represents a true change in the cells in a seborrheic wart. A large number of age-related keratomas may be a sign of cancer of internal organs.
Typically, seborrheic keratoses are treated for cosmetic reasons or because they become itchy and irritating. If the growths, especially large and warty ones, are injured (rubbed against clothing, touched by something), they may bleed or become inflamed.
Diagnosis of the disease is usually made through a clinical examination. This type of wart is difficult to distinguish from skin cancer without histological examination. Therefore, very dark lesions that have changed in some way or that are growing rapidly require a biopsy to confirm the diagnosis and rule out the possibility of cancer. Darker lesions should also be checked by a doctor to make sure they are not melanoma.
Treatment of warts in St. Petersburg
Treating warts requires a lot of patience. Warts may appear and disappear for no apparent reason or for reasons that are difficult to identify. High infectivity and autoculation of warts are arguments in favor of removal.
There are many different treatment methods. Therapeutic choices differ depending on the type of wart, its location, depth, number and extent of the affected area of skin.
Treatment for warts can produce very different results. Some warts respond to treatment while others do not, even if it is given to the same person.
Treatment often requires repetition over several weeks, months and in extreme cases even years before success is achieved. But in any case, wart removal should be performed in a clinic by a dermatologist. Self-medication is highly discouraged, as the consequences may be irreparable.
The most gentle and universal ways to get rid of warts of all types are laser and radio wave therapy.
Let's sum it up
Mucous fibroids on the inside of the cheeks, gums, lips, and tongue grow very slowly and do not cause severe discomfort. They do not pose a danger to the patient, but the problem must be eliminated as early as possible. The fact is that a benign seal in the oral cavity with regular trauma can degenerate into a malignant one, and the oncological process requires serious therapy and is extremely dangerous to life and health.
It is impossible to get rid of the disease using traditional methods. It is important to undergo high-quality dental diagnostics and consult with specialists. In most cases, surgical excision is indicated, but with small growths, the absence of severe symptoms and the elimination of provoking factors, there is a possibility of rapid tissue restoration without external influence.
There is no need to worry if the doctor has decided to undergo surgery. Modern clinics practice laser or radio wave removal on an outpatient basis. These are the most gentle and highly effective methods. An extremely important point in a positive prognosis for the treatment of dental fibroids is an early visit to a doctor and proper excision by an experienced physician.
Laser wart removal
Today, laser surgery is one of the best ways to get rid of warts. This is a painless and safe procedure that can be used in areas of maximum sensitivity. Laser removal of tumors is very effective: the likelihood of relapse is minimal. This is significantly influenced by the severity of the disease.
Warts are removed by layer-by-layer cauterization of the affected area, thanks to which the doctor controls the depth of the effect. At the same time, the laser beam cauterizes the blood vessels, thereby preventing bleeding at the site of exposure.
Three methods of laser coagulation are common:
- Carbon dioxide (CO2) laser. Procedures using this laser are more painful. Although the CO2 laser seals the blood vessels, it also kills the wart tissue. In this process, there is a possibility of damage to healthy tissue. Wound healing usually takes longer, and scar formation is possible. The efficiency is about 70%.
- Erbium laser. It is characterized by a shorter wavelength. The likelihood of scar formation after healing is significantly reduced.
- Pulsed dye laser. This laser more effectively seals the blood vessels that feed the wart. It does not damage much of the healthy tissue like a CO2 laser does. It is also the only type of laser approved for use on children. The effectiveness of this treatment method is about 95%.
| Advantages | Flaws |
| Minimum likelihood of scar formation (depending on the degree of neglect of the pathology) | High price |
| Fast tissue healing | |
| High efficiency of the method | |
| Minimal damage to healthy tissue | |
| Speed of the procedure |
Wart removal is performed under local anesthesia. A crust remains at the cauterization site, which disappears within 14 days. After the procedure, the patient quickly returns to his normal lifestyle, provided that all doctor’s recommendations are followed.