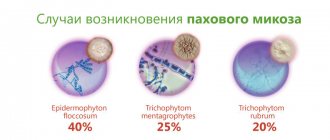
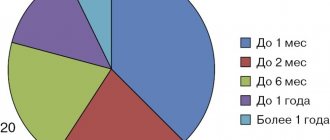
Types of fungal infections
Three types of fungi live in the human body:
- yeast;
- moldy;
- domiformes.
Only the first variety is considered opportunistic: such microorganisms cause harm only if immunity is reduced and metabolism is disrupted. As for the other two types of fungi, they are always dangerous to health.
Depending on the pathogen, fungal infections such as:
- Candidiasis. Yeast fungus of the genus Candida affects the skin and mucous membranes.
- Trichophytosis, or ringworm. The pathogenic microorganism trichophyton causes damage to hair, nails, and skin.
- Dermatophytosis. A fungus of the genus Arthodermataceae parasitizes the scalp, skin and nails.
- Keratomycosis. The causative agents are Aspergillus and Actinomycetes. The stratum corneum of the skin suffers from them.
Fungal diseases can affect fingers and toes, nails, hands, feet, hair and so on. Pathogens also penetrate the vagina, throat, intestines and other internal organs.
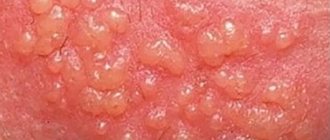
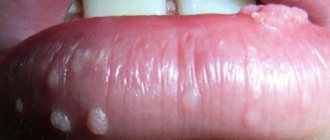
Different types of mycoses have special symptoms, but they also have characteristic manifestations. At the beginning of the disease, the affected area peels off, turns red and becomes inflamed. Then small bubbles appear. They burst, and in their place erosions form, which itch and hurt. The skin becomes loose and even begins to peel off.
Causes of age-related colpitis
If in young women the inflammatory process of the vagina develops mainly as a response to a pathogenic infectious agent, then age-related vaginitis is associated primarily with hormonal changes. Against the background of a sharp decrease in estrogen levels, rapid depletion of the vaginal mucous membranes occurs. This process is accompanied by a significant change in the quantitative composition of the natural microflora of the vagina. First of all, the number of vaginal bacilli and lactobacilli that produce lactic acid is reduced. The acidity of the mucous membranes is lost and the pH of the environment almost doubles to pH 5.0-7.0.
The acidic reaction of the membranes of the genital organs serves as the main deterrent for the development of opportunistic vaginal flora - Candida yeast, Escherichia, E. coli, etc. When this protective mechanism is lost and the mucous membranes begin to deplete, all these normal inhabitants of the vagina begin to actively grow and multiply , causing inflammation. In some cases, pathogenic microorganisms - Trichomonas, ureaplasma, chlamydia, etc. - can also serve as the root cause of the infectious-inflammatory process.
It is important to note that the described form of vaginitis sometimes affects young women if they have the following risk factors:
- immunodeficiency states;
- endocrine pathologies – diabetes mellitus, obesity, thyroid disorders;
- patients who have had their ovaries removed;
- women who have undergone radiation and radiotherapy.
Failure to comply with the rules of intimate hygiene and wearing tight synthetic underwear are also factors that provoke a violation of the composition of the vaginal microflora.
Why are fungal infections dangerous?
Mycoses have a variety of symptoms. Almost always there is severe itching, an unpleasant odor, and possible pain.
However, the main danger is that fungi quickly spread throughout the body and affect new areas. A systemic infection cannot be ruled out when pathogens penetrate deeply into tissues and organs. The patient experiences weakness, pain, suffers from digestive disorders, toxicosis, and skin rashes.
Without the help of a specialist, the disease worsens and becomes chronic with frequent exacerbations. In the most severe cases, sepsis and death cannot be ruled out. The sooner you see a doctor, the easier it will be to get rid of pathogenic flora.
Home remedies cannot cure the infection. At best, it will go into “sleep” mode. The patient is not able to independently identify the pathogen and, accordingly, choose the correct treatment method.
Treatment
Medication method
There are 2 options for using antifungal drugs:
- external use at the site of pathology localization,
- oral medication.
The question of how to treat inguinal epidermophytosis is decided based on concomitant diseases. Taking medications orally occurs when, in addition to mycosis in the groin area, there is a fungus on other parts of the body (on the nails, on the feet). Information about the drugs recommended in such cases is provided in the table.
Doctor's advice
The causes of a rash in the groin area can be very different: bacteria (for example, erythrasma), contact dermatitis (for example, on the material of clothing, underwear), eczema, and so on. Therefore, it is very important to see a doctor when a rash is detected in order to determine the true cause of the disease and quickly help the skin.
Inna Zhikhoreva Dermatologist, Venereologist, Hair diseases
| Notes on use | Terbinafine tablets (250 mg per tablet) | Itraconazole capsules (100 mg per capsule) |
| Daily intake of the drug | 1 tablet once after meals | 2 times 2 capsules |
| Duration of treatment | 2-4 weeks | 1 Week |
| Contraindications | vascular pathology of the extremities, metabolic disorders, the presence of tumors, liver failure | heart pathology (treated by a cardiologist) |
| special instructions | lack of improvement after 2 weeks is a reason to consult a doctor to confirm the correctness of the identified causative agent of the disease | use caution in case of renal pathology, peripheral neuropathy and liver disorders |
| Side effects | diarrhea, dizziness, abdominal pain | hair loss, heart failure, hypokalemia, diarrhea, dizziness, abdominal pain |
The drugs indicated in the table disrupt the cell membrane of fungi, which causes their death. It is important to avoid interruptions in taking medications. Otherwise, there is a surge in the disease.
If inguinal athlete's foot is not accompanied by other mycotic lesions on the body, treatment of the patient is limited to antifungal agents for external use.
The already mentioned Terbinafine is available not only in tablets, but also in the form of 1% ointment or cream. The active substance of the drug is good at destroying pathogens of mycoses, therefore it tops the list of drugs prescribed by dermatologists for the treatment of inguinal athlete's foot.
The affected area of the groin area is washed and dried. Twice a day, apply a thin layer of ointment (or cream) and rub in gently. The area of application is not limited to just the affected area; the medication is also applied beyond the “cord” by about 2-3 cm. Cure occurs in about a week.
In the line of antifungal drugs, another medication occupies an advantageous position - Termicon (generic Terbinafine).
The medicine is available in the form of a spray, thanks to which it:
- does not cause a greenhouse effect (unlike fat-based ointments);
- dries affected skin areas;
- not only fights fungal infection, but also has anti-inflammatory and antipruritic effects.
The method of using the spray is similar to using ointment and cream.
Treatment of inguinal athlete's foot (even advanced ones) does not involve large material costs. Each of the drugs mentioned is characterized by affordability. This thesis is confirmed by information from the table.
| Drug name | Release form | Price range (RUB) |
| Terbinafine | tablets (250 mg) | 200 – 300 |
| Terbinafine | ointment 1% (15 g) | 70 – 100 |
| Terbinafine | cream 1% (15 g) | 70 – 100 |
| Thermikon | spray (15 ml) | 200 – 300 |
| Itraconazole | capsules (100 mg) | 300 – 400 |
It is not difficult for an experienced dermatologist to identify the disease when examining a patient. However, given the self-medication often practiced by patients (the use of various ointments, the use of traditional methods, etc.), it would be more competent to conduct a cultural study of the scales. This is sowing on a special medium, which takes about a month. Unlike the conventional microscopic method, cultural analysis is more informative.
Inna Zhikhoreva
Dermatologist, Venereologist, Hair diseases
Athlete's inguinal athlete is not a cause for concern. It is easy to diagnose and just as easy to treat, which is why treatment occurs at home.
To get healthy men back on track faster, do not self-medicate. Thus, taking anti-inflammatory drugs (instead of antifungals) for inguinal athlete's foot relieves itching and some other obvious symptoms. At the same time, the causative agents of fungal infection are not destroyed, but lead a secretive lifestyle in order to expose themselves at the most inopportune moment.
This article has been verified by a current qualified physician, Inna Zhikhoreva, and can be considered a reliable source of information for site users.
Rate how helpful this article was
4.4 18 people voted, average rating 4.4
Did you like the article? Save it to your wall so you don’t lose it!
Why do they trust us to treat fungal diseases?
The medical department employs qualified dermatovenerologists. Our doctors - V. A. Malashenko and R. A. Guseinov - specialize, among other things, in mycology, so they accurately diagnose and prescribe optimal treatment.
Accurate identification of the pathogen plays an important role in removing fungus. We perform tests that reveal:
- presence of a pathogen;
- its appearance;
- quantity;
- sensitivity to certain antifungal drugs.
Fungi are studied using various methods - microscopy, PCR, inoculation on nutrient media. The availability of options allows you to choose the most suitable one for a particular patient.
Based on the results of the analysis, our specialists create a comprehensive treatment regimen. As a rule, it includes oral antifungal drugs, as well as topical agents. By following doctors' prescriptions, you will completely get rid of the infection, and the affected areas will restore their integrity.
An appointment with a dermatovenerologist at the clinic on Tretyakovskaya costs 1,500 rubles. We work at convenient times, seven days a week.
Diagnosis and treatment of age-related colpitis in women
A gynecologist can make a diagnosis based on a standard examination and determination of the pH level of the vagina. Bacterioscopic and bacteriological examination of a smear helps to determine the specific pathogen and its sensitivity to antibacterial drugs. An additional diagnostic measure is an extended vaginal colposcopy.
The main direction of treatment for colpitis in older women is hormone therapy. Gynecologists prefer to prescribe natural estrogens. Local application of antibacterial ointments and gels is also prescribed, which are selected individually, taking into account the sensitivity of the identified pathogen. Baths with decoctions and infusions of herbs that have anti-inflammatory and antibacterial effects have a positive effect. Additionally, a set of measures for general strengthening therapy is being formed, which includes taking multivitamins and normalizing the diet.
Experienced gynecologists of the multidisciplinary medical center of the European level of service NEOMED will help diagnose and treat age-related colpitis in women.
Make an appointment with a gynecologist
Treatment of fungal skin diseases
The cause of dermatomycosis is infection by pathogenic microorganisms. For a person to get sick, contact with infected objects is enough - shoes, towels, washcloths, and so on. The risk of infection is high in people who suffer from sweating feet, varicose veins, diabetes, endocrine disorders and other diseases that reduce immunity.
In our “Polyclinic +1”, appointments are conducted by first category doctors V. A. Malashenko and R. A. Guseinov. They have specialties such as dermatology and mycology. Each of these doctors has many years of practical experience, so they are able to cope with the most difficult cases.
We offer several types of tests for pathogenic flora. Scrapings from the affected area are studied using various methods, including:
- microscopy;
- PCR;
- sowing on nutrient media.
These studies will allow you to identify the fungus, determine its type, and find out what drugs it reacts to.
After this, our doctors draw up a treatment plan for the fungal infection. We practice an integrated approach, so we combine tools that solve different problems:
- destroy harmful microorganisms,
- strengthen the immune system;
- heal the skin.
The duration of therapy depends on the severity of the disease, the body’s resistance and other factors. In any case, our specialists monitor the process and, if necessary, adjust the assignments.
Recommendations for the prevention of candidiasis in the groin
Genital candidiasis is one of those diseases whose development is much easier to prevent.
What then to do with long and rather expensive treatment, as well as get rid of side effects.
To prevent infection, people should follow the following recommendations:
- When having sex, follow basic safety rules, without refusing to use condoms, especially if you are not completely confident in your partner’s health
- Always remember personal hygiene by not using other people's items from this area
- When visiting public swimming pools and baths, rinse thoroughly in the shower after sessions
- When taking glucocorticosteroids, antibiotics and immunosuppressants, carefully observe the dosage and duration of therapy as recommended by the attending physician
- promptly treat identified diseases of the genital organs, not only infectious, but also of other origins
- devote time to hardening the body so that the immune system does not weaken under the influence of stress and other negative environmental factors
- treat diseases of the endocrine system in a timely manner; if you have diabetes, make efforts to take the disease under control
Unfortunately, doctors note, even following these simple recommendations cannot protect against candidiasis 100%.
However, if you follow these recommendations, the likelihood of encountering the disease during your life will be significantly reduced.
Treatment of genital fungal diseases
Both women and men are susceptible to fungal genital infections. The causative agents of the disease are Candida yeast fungi. They are present in minimal concentrations in the body of almost 80% of people. Under unfavorable conditions, pathogens multiply and infect the genitals.
Factors that activate the growth of fungi are:
- metabolic failure;
- uncontrolled use of antibiotics, hormonal drugs;
- injuries and operations;
- constant stress;
- climate change;
- neglect of personal hygiene.
Pregnant women and people with endocrine, sexually transmitted and infectious diseases are also at risk.
In patients of both sexes, genital mycosis is manifested by symptoms such as:
- skin irritation and redness;
- unbearable itching of the mucous membranes;
- pain during urination or sexual intercourse.
Erosions, spots, and ulcers often appear on the genitals.
Women note a cheesy discharge that has an unpleasant odor. The labia become red and swollen. Constant itching leads to irritability, fatigue, and insomnia.
Fungal diseases of the penis are accompanied by swelling of the foreskin and redness of the urethral sponges. A thick white coating, redness, and erosion appear on the head. The skin of the penis may become cracked, and sometimes there is growth of lymph nodes in the groin. After a night's sleep, there is discharge from the urethra.
Genital fungal diseases themselves cause great discomfort. However, they are also dangerous due to their complications. Self-medication or failure to consult a doctor in a timely manner risks that the infection will penetrate the internal organs of the genitourinary system. This will result in various diseases, in particular infertility.
When may irritation appear in the intimate area?
The cause of irritation in the intimate area can be a variety of circumstances. Even habitual actions that at first glance do not carry any risk can lead to a feeling of discomfort. The most common cases when a woman may experience irritation in the most delicate area:
- after shaving
. Removing unwanted hair with a razor often leads to microtrauma. Such wounds become entry points for pathogens, and irritation develops as a result of infection. A machine with dull blades is especially dangerous in this regard. In this case, the likelihood of cuts and infection increases significantly. Another risk factor related to shaving is using the wrong product to help remove unwanted hair (such as soap or shower gel); - after intimacy.
In some cases, intimate intimacy itself becomes a cause of irritation due to injury to the mucous membrane of this delicate area. But most often, irritation develops when there is insufficient lubrication and dryness of the mucous membrane, when using lubricants with flavors, or if contraception is used (suppositories, vaginal tablets, condoms with flavored lubricant, etc.), to which a woman has increased individual sensitivity or is allergic; - after taking antibiotics
. In many cases it is impossible to do without antibiotic therapy. But these drugs cannot distinguish between harmful and beneficial bacteria and strike both the former and the latter with equal force. However, the microflora of the intimate zone, which consists of many types of beneficial bacteria, plays a very important role for women's health. When their number decreases, other microorganisms begin to predominate in the microflora, in particular Candida fungi, which can cause inflammation and severe discomfort in the intimate area.
How to cure a fungal genital infection?
Dermatovenerologists at the Polyklnika+1 clinic are fluent in the specialty of mycology. That is why you will receive qualified diagnostics and treatment from us.
Doctors of the first category V. A. Malashenko and R. A. Guseinov use modern methods to detect mycosis at an early stage, even if it is disguised as a bacterial STI. We carry out research:
- an imprint from the glans penis, labia, foreskin, as well as scraping of scales from skin rashes using microscopy;
- smear from the vagina, urethra, cervical canal;
- Fungal DNA in mucosal scrapings (PCR method).
The results of these tests are ready in half an hour or the next day. In addition, within seven days you will receive a response to sowing the biomaterial on nutrient media. Such a study allows us to determine the type of pathogen, its quantity and the degree of sensitivity to drugs.
Guided by the results of the research, specialists at the Tretyakovskaya clinic are drawing up a comprehensive treatment regimen for fungal infections of the genital organs. They take into account factors such as:
- severity of inflammation;
- damage to the mucosa;
- presence of edema.
In accordance with this, the patient is prescribed antifungal, antibacterial, hormonal, wound-healing drugs - in the form of tablets, ointments, intravenous injections. If necessary, immunomodulators and probiotics are prescribed.
The treatment process takes from a week to several months, depending on the severity of the disease. Thanks to the experience and knowledge of our doctors, therapy gives excellent results and minimizes the possibility of relapse.
Is sex acceptable during candidiasis treatment?
Often men and women who have received a diagnosis from a doctor wonder whether sex is possible during treatment.
Doctors draw the attention of their patients to the fact that sex will have to be excluded for the entire period of therapy.
This is due to several factors.
Firstly, it is recommended to undergo therapy not only for the first one of the couple to seek help, but also for his sexual partner.
Secondly, if you do not refuse sexual contact, re-infection will occur as soon as the therapy is completed.
It would seem that a condom should provide protection from the transmission of infection.
This is actually true, but it is important to remember that candidiasis can affect not only the genitals, but also the skin around them.
And the skin is often not covered with a contraceptive, which means there is no protection in this area.
We also must not forget that the condom may break or be initially incorrectly selected.
Then the degree of protection against infection decreases even more.
Fungus in men's groin
Male groin fungus is an infection of the skin of men caused by mainly two types of fungi. These are epidermophytes and trichophytes.
A man can become infected with a fungus:
- From a sick man to a healthy man
- Through objects contaminated with scales of a patient with fungi
Infection often occurs through towels, bedding, medical instruments, and clothing.
Infection is promoted by:
- Frequent skin trauma
- Fever
- Sweating of the inguinal folds and scrotum
- Physical exercise
- Tight underwear
A large role in the spread of fungus in men in the groin is played by frequent asymptomatic infection of the scrotum by the fungus.
Fungus in the groin of men, caused by epidermophytes, is isolated into a separate form - inguinal epidermophytosis.
What appears in men with athlete's foot inguinal?
With inguinal epidermophytosis in men, slightly scaly, sharply demarcated lesions appear in the form of red spots. The color of the spots is red or reddish-brown. The spots gradually grow along the periphery and “recover” in the center. As a result, ring-shaped figures are formed. They extend beyond the inguinal folds.
Along the periphery of the spots there is a ridge of small bubbles or nodules.
The skin of the scrotum is affected very often. As a rule, it turns red and thickens.
If left untreated, this form of fungus in men's groin lasts for years. Exacerbations occur in the hot season. They are caused by sweating and friction.
Fungus in the groin of men caused by trichophytons
Fungus in the groin of men caused by trichophytons has a chronic course from the very beginning. Most often the inguinal and intergluteal folds are affected.
Unlike athlete's foot, this fungus often spreads to other folds and surrounding skin.
These fungal diseases are similar in their manifestations. Severe itching is often observed.
Fungus in the groin of men can be difficult to distinguish from erythrasma. Tests help with this - scraping for fungus and culture for bacteria.
Candidiasis in the groin: methods of diagnosis
Before starting treatment for groin candidiasis, it is necessary to confirm the diagnosis.
This is not always easy, especially if the patient may have pathologies that resemble a candida infection in their symptoms.
First of all, an inspection is carried out.
Based on the results, the doctor evaluates the rash, the severity of swelling and other symptoms.
After this, the question of how to differentiate candidiasis using laboratory methods is resolved.
First of all, the patient is recommended to undergo a smear test.
In women, a smear is taken quite easily.
Men will have to endure several unpleasant minutes.
However, the effectiveness of collecting material in terms of diagnostics is high, and therefore you should not refuse.
The resulting smear can be examined in several different ways.
Most often, in addition to microscopy, sensitivity culture is performed.
Thanks to him, the doctor receives information about what medications can be used to treat the disease, and also confirms the diagnosis.
Additionally, PCR tests and scrapings are often done.
Additional research is especially important in doubtful cases.
When a patient, for example, also has symptoms of inguinal athlete's foot or an allergic reaction, and it is necessary to differentiate the diseases from each other.
In children, it is especially important to pay attention to analysis.
Diaper rash and allergies in the groin area are similar to candidiasis.