Downloads
M. Gomberg.
There are enough reasons (636.66 Kb)To download the file, use the built-in capabilities of your browser. The PDF file can be read using a free program or built-in browser tools. Special project of the Medical Bulletin: vaccine prevention. Human papillomavirus
Additional materials
HPV vaccination. 2016 ACS Recommendations
Why is the HPV vaccination necessary?
General information
Human papillomavirus (HPV) is the most common viral infection of the genital tract. HPV is a group of viruses that is extremely common throughout the world. There are more than 190 types of this virus, of which at least 13 lead to cancer (these are known as high-risk types). The human papillomavirus is transmitted primarily through sexual contact, and most people become infected soon after they become sexually active. Two types of HPV (16 and 18) cause 70% of all cases of cervical cancer (CC) and precancerous conditions of the cervix.
Chance of getting sick
The human papillomavirus is transmitted primarily through sexual contact, and most people become infected soon after they become sexually active. But penetrative sex is not necessary to transmit the virus. Skin-to-genital contact is a well-established route of transmission of human papillomavirus infection. Risk groups for HPV infection are children and adolescents aged 15-18 years.
Cervical cancer develops as a result of sexually acquired infection with certain types of HPV. Risk factors for developing cervical cancer: first sexual intercourse at an early age; multiple sexual partners; immunosuppression (eg, people living with HIV are at increased risk of acquiring HPV and are infected with a wider range of HPV types).
Symptoms and nature of the disease
Most HPV infections do not cause symptoms or illness and go away on their own (about 90% resolve within 2 years). However, persistent infection with certain types of HPV (most often types 16 and 18) can lead to the development of precancerous conditions. Without treatment, these conditions can develop into cervical cancer. Today, cervical cancer is the most common disease associated with the human papillomavirus. Cervical cancer is the fourth most common cancer in women, and the seventh most common cancer overall, with an estimated 528,000 new cases worldwide in 2012.
Symptoms of CC usually appear only in advanced stages of cancer and may include the following:
- Irregular, intermenstrual (between periods) or abnormal vaginal bleeding after sexual intercourse;
- Pain in the back, legs or pelvic area;
- Fatigue, weight loss, loss of appetite;
- Unpleasant sensations in the vagina or discharge with an unpleasant odor;
- One swollen leg.
In later stages, more severe symptoms may appear.
Human papillomavirus infection is also implicated in 20-90% of cases of squamous cell cancer of the anus, oropharynx, vulva, vagina and penis. It is estimated that up to 90% of all anal cancers are caused by HPV-16 and HPV-18, and 40% of vulvar cancers, which occur mainly in older women, are associated with HPV-16.
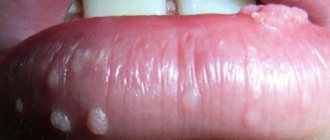
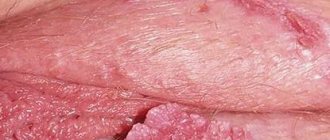
Low-risk HPV infections cause anogenital warts in men and women (genital warts or venereal warts). The average time between infection with HPV types 6 or 11 and the development of anogenital warts is 11–12 months in men and 5–6 months in young women 16 . Anogenital condylomas are difficult to treat.
HPV-6 and HPV-11 can also cause a rare condition known as recurrent respiratory papillomatosis (RRP), in which warts form in the larynx or other parts of the respiratory tract. RRP is observed mainly in children under 5 years of age (juvenile RRP) or in people in their third decade of life (adult RRP). In rare cases, women with genital HPV infection can pass the virus to the baby during childbirth. Untreated RRP can lead to serious problems due to airway obstruction.
Complications after an illness
It has been established that cervical cancer in 100% of cases is caused by oncogenic types of human papillomavirus (HPV). In women with a normal immune system, cervical cancer develops within 15-20 years. In women with weakened immune systems, such as those with HIV infection, if left untreated, it may take only 5-10 years for it to develop. Although data on anogenital cancers other than cervical cancer are limited, growing evidence links human papillomavirus to cancers of the anus, vulva, vagina and penis. Although these cancers are less common than cervical cancer, their association with HPV makes them potentially preventable through the same primary prevention strategies as for cervical cancer.
HPV types that do not cause cancer (especially types 6 and 11) can cause genital warts and respiratory papillomatosis (a disease in which tumors grow in the airways leading from the nose and mouth to the lungs). Although these conditions very rarely result in death, they can often lead to illness. Genital warts are widespread and highly infectious.
Human papillomavirus HPV and cervical cancer
Human papillomavirus (HPV) is a DNA virus of the Papillomaviridae family. This family includes common and genetically diverse viruses that infect and damage epithelial cells (skin, mucous membranes of the anogenital area, oral cavity).
More than 130 HPV genotypes are known. According to clinical classification, they are divided into cutaneous and anogenital types of papillomaviruses. It is the anogenital types of HPV that cause damage to the mucous membranes of the vagina and cervix. The most harmless of these diseases are benign genital warts, the most dangerous is cervical cancer.
Human papillomaviruses are transmitted through sexual contact. With the onset of sexual activity, the vast majority of women become infected with this virus. It should be taken into account that the risk of HPV infection depends on the number of sexual partners and on the sexual behavior of the only partner (the prevalence of HPV in men is approximately equal to the prevalence in women).
Human papillomavirus infection itself is not a disease. After 6-18 months, in ~80% of infected women, the virus leaves the body on its own, without any treatment, without causing illness (spontaneous elimination). And only a small percentage of women with chronic (persistent) infection caused by highly oncogenic HPV genotypes may develop cervical cancer after 10-20 years. It seems that there is enough time for successful diagnosis and treatment, but there is no need to relax.
Human papillomavirus infection is very insidious, and the precancerous changes associated with it, as a rule, not only do not cause any concern or discomfort, but are often not detected during a routine gynecological examination.
Therefore, to detect human papillomavirus infection, an HPV test using the polymerase chain reaction (PCR) method is used. The HPV test is a reliable doctor’s assistant: detection of papillomavirus and determination of its genotype allows you to determine further tactics for the management and treatment of a woman.
It should be taken into account that the identification of HPV of a high carcinogenic risk group in women is not the basis for making a diagnosis of a malignant tumor, but serves as a reason for further examination, more intensive monitoring and, if necessary, treatment of precancerous changes in the cervical mucosa.
The outcome of HPV infection depends on the genotype of the virus. All papillomaviruses are divided into groups according to “harmfulness” or “oncogenicity”. HPV polymerase chain reaction (PCR) tests detect all common and clinically significant HPV genotypes.
The low carcinogenic risk group includes HPV genotypes 6 and 11: they can cause genital warts and mild dysplasia. Analysis for HPV genotypes 6 and 11 is used for differential diagnosis with diseases of non-papillomavirus etiology and when examining pregnant women to assess the risk of developing laryngeal papillomatosis in newborns.
- Human papillomavirus 6/11, qualitative DNA determination, PCR
Genotypes 16 and 18 of papillomaviruses most often lead to cervical cancer. They, together with types 31, 33, 35, 39, 45, 51, 52, 56, 58, 59 and 68, are included in the group of high carcinogenic risk. When conducting tests for human papillomavirus, it is these genotypes that you need to pay special attention to. The most important is DNA analysis of HPV types 16 and 18, especially if their con) is high. And the oncogenic potential of types 51 and 56 is not so great, so they are less dangerous, even if they are present in relatively large quantities in the HPV test.
- Human papillomavirus 16/18, qualitative DNA determination, PCR
- Human papillomavirus 16/18, DNA quantification, PCR
- Human papillomavirus of high carcinogenic risk (16, 18, 31, 33, 35, 39, 45, 51, 52, 56, 58, 59, 68), total qualitative DNA determination, PCR
- Human papillomavirus of high carcinogenic risk (16, 18, 31, 33, 35, 39, 45, 51, 52,56, 58, 59), qualitative determination of DNA indicating the type of virus
- Human papillomavirus of high carcinogenic risk (16, 18, 31, 33, 35, 39, 45, 51, 52, 56, 58, 59, 68), total DNA quantification
- Extended HPV test (with determination of the amount and type of virus)
You can get tested for HPV in women using the PCR method (HPV test) yourself, without a doctor’s referral. If HPV infection is not detected (negative HPV test result), then the risk of developing cervical cancer is low. But you should remember that if you continue to be sexually active, the risk of HPV infection remains.
If the result of the HPV test is positive, HPV of high carcinogenic risk is detected, it is necessary to do an extended study to clarify the genotype of the virus (HPV analysis - typing) and the “viral load” (human papillomavirus - quantitative analysis). Then you need to contact a gynecologist for a colposcopy - an examination of the cervix under magnification using a special device - a colposcope.
All additional tests for human papillomavirus and other studies must be carried out as prescribed and under the supervision of a physician.
If damage to the cervical mucosa is detected at an early stage, preceding cancer, then treatment is more effective and has virtually no side effects. If no pathological changes are detected in the cervical mucosa, then there is no need for treatment: most likely, the body will cope with the virus on its own.
However, after 1 year, it is necessary to undergo repeated HPV testing and, if the virus is still present, to be examined again by a gynecologist.
Analysis for human papillomavirus (HPV) by PCR and cytological studies.
In Russia, the compulsory health insurance (CHI) system includes a cytological examination - “smear for oncocytology”. Are HPV tests necessary then?
The basis of modern screening programs for the early detection of cervical cancer is the Papanicolaou cytological examination (PAP test, Papanicolaou staining). Unfortunately, not all Russian medical institutions use this technique; very often other, less advanced methods of preparing (staining) a cytological smear are used.
In addition, it is important to know that the cytological method is not an analysis for the human papillomavirus. Cytology “does not see” the virus itself, but reveals epithelial cells that have already been changed under its influence, that is, clinical and subclinical forms of HPV infection. The cytological test also has very significant disadvantages - low sensitivity, subjectivity of interpretation and dependence of the result on the quality of the cytological smear.
That is why traditional cytological screening is characterized by a large number of false-negative and indeterminate results requiring repeated studies.
To reduce the possibility of errors, cytological tests have been improved - the liquid cytology method has been introduced. Liquid-based cytology is a new technology for preparing cell samples from the cervix for cytological examination. The advantages of this method are a reduction in the number of inadequate smears and artifacts, and the ability to avoid contamination of samples with inflammatory exudate and red blood cells, which ensures high quality cytological preparations. Today, it is this method of cytological screening for cervical diseases that is recommended by WHO (World Health Organization) as the “gold standard” for the study of cervical smears.
- Pap test liquid
According to the latest international and domestic recommendations, the combined use of HPV analysis (HPV PCR test) and cytological examination (PAP test) is the preferred method for the early detection of cervical cancer in women over 29 years of age. Such screening must be carried out regularly - once every 3 years.
- HPV-PAP test (set of tests: HPV extended with determination of the amount and type of virus + PAP test)
- HPV-PAP test liquid (set of tests: HPV extended with determination of the amount and type of virus + PAP test)
Treatment
CC screening is testing for precancerous conditions and cancer among women who have no symptoms and feel completely healthy. If screening detects precancerous conditions, they can be easily treated and thus prevent the development of cancer. Screening can also detect cancer at an early stage with a high chance of cure.
Given that precancerous lesions develop over many years, it is recommended that every woman aged 30–49 years be screened at least once in her life, preferably more often. Screening is only effective in reducing cervical cancer mortality if a significant number of women participate.
There are currently 3 different types of screening available:
- Routine Papanicolaou (Pap) test and liquid-based cytology (LBC);
- Visual inspection using acetic acid;
- Testing for high-risk HPV types.
Developed countries have programs that provide screening opportunities for women, which allows most precancerous conditions to be detected at stages when they can be easily treated. Early treatment for human papillomavirus can prevent up to 80% of cases of cervical cancer in these countries.
In developing countries, limited access to effective screening means that the disease is often only detected in advanced stages, when symptoms have developed. In addition, treatment of the disease at such advanced stages is of little promise, which leads to high mortality rates from cervical cancer in these countries.
“Effective treatment for HPV” - false or true?
It is important to understand that there are no serious and complete studies on any of the above drugs - randomized, double-blind, placebo-controlled trials. Advertising and laudatory publications and studies with non-representative samples are posted only on manufacturers’ websites and Russian-language resources. Apart from the CIS countries, these funds are not registered and are not used anywhere.
Many Russian gynecologists claim that drugs with unproven effectiveness successfully treat HPV: the test for the virus becomes negative after one or several courses. But this result is not a merit of the treatment; it means that the infection was transient and would have gone away on its own, even without the unnecessary drug and financial burden.
World practice
The US Center for Disease Control writes that specific therapy for HPV is not recommended. WHO in its fact sheet only talks about the need to treat the consequences that HPV can cause: cervical cancer, anal or genital warts. In men, oncogenic types of HPV can cause cancer of the rectum and penis.
In the modern world, there is no drug therapy, but much attention is paid to vaccination.
HPV vaccination
Two vaccines have undergone clinical trials and are registered on the market:
- Gardasil - protects against HPV 6, 11, 16, 18;
- Cervarix - protects against HPV types 16 and 18.
The drugs are very expensive (the price of one injection is about 6,000 - 10,000 rubles), so only developed countries can afford mass vaccination.
Ideally, all adolescents aged 11-12 years, regardless of gender, should be vaccinated (twice within six months) and adults under 26 years of age (three times after 14 years of age within six months). Russian vaccine instructions recommend three-time vaccination at any age.
Separately, it is worth mentioning that the American Alliance of Immunologists recommends vaccination against HPV for HIV. WHO, clinical studies of the Canadian Institute of Health Research and other publications speak about the effectiveness of vaccination of HIV-positive girls.
When should you get tested for HPV?
HPV testing is prescribed to women over 30 years of age with abnormal cytology or histology results. It’s just pointless and costly to carry it out like that. The results of the PAP test, together with the HPV test, help determine the correct interval before repeat cytological examination or colposcopy.
A positive HPV test does not mean cancer, it only allows you to make a rough prognosis; Moreover, the virus is not the only risk factor for cervical cancer.
The HPV test should not be used in large numbers - it is an additional (and expensive) screening method.
Result:
- There is no proven antiviral therapy for HPV, nor are there drugs that strengthen the immune system.
- It is not HPV that is treated, but its consequences: precancerous conditions and cervical cancer, neoplasms on the skin and mucous membranes. The treatment is not medicinal, but surgical: laser, cryodestruction, surgery.
- There is no need for everyone to get tested for HPV.
Effectiveness of vaccination
Clinical trial results indicate that the two vaccines available today are safe and very effective in preventing infection with HPV 16 and 18. Both vaccines are more effective if vaccinated before exposure to human papillomavirus. Therefore, it is preferable to vaccinate before the first sexual contact. Vaccines do not treat HPV infection or HPV-related disease (such as cancer).
Some countries have introduced HPV vaccination for boys because it prevents genital cancer in both men and women, and one available vaccine also prevents genital warts in both men and women. In addition, vaccinating boys serves to prevent the circulation of HPV in the adolescent and young adult population. WHO recommends that girls aged 9–13 years be vaccinated as it is the most cost-effective public health intervention against cervical cancer.
HPV vaccination is not a substitute for cervical cancer screening. In countries where the HPV vaccine has been introduced, the development of screening programs may also be necessary. By the end of 2013, the human papillomavirus vaccine had been introduced in 55 WHO countries.
Modern mathematical models show that when girls aged 12-13 years are covered with a full course of primary immunization (3 doses) with a vaccine against human papillomavirus infection, it is possible to predict a reduction in the risk of developing cervical cancer by 63%, cervical intraepithelial neoplasia of the third severity (precancer) - by 51 %, cytological disorders in age cohorts under 30 years – by 27%.
Causes of papillomas
Papillomavirus DNA can be functionally inactive and activated under the influence of:
- smoking,
- hormonal disorders,
- concomitant STIs, and, above all, genital herpes, the causative agent of which is HSV-2.
Infection of the genital organs occurs in the presence of microtraumas in the genital area (mechanical trauma, bacterial microdamages, etc.), and it should be taken into account that the urethra, seminal fluid and prostate secretions can serve as a reservoir.
The incubation period for genital warts usually varies from several months to several years, and in most cases the infection is subclinical. Progression of a high oncogenic risk infection into cutaneous dysplasia and carcinoma in situ usually occurs within 5 to 30 years and rarely within a period not exceeding 1 year. Human papillomavirus infection of the genitals is often multifocal and associated with more than one type of human papillomavirus, as well as other pathogens of STIs In most cases, genital human papillomavirus infection remains unrecognized. Genital infection is highly contagious and acquired during the first few sexual contacts; Infection occurs during a single sexual contact in approximately 60% of cases. In 65-70% of cases, papillomas (warts) are detected in both sexual partners.
The likelihood and frequency of developing a genital infection largely depends on a person’s sexual behavior. Risks increase when:
- early onset of sexual activity,
- frequent change of sexual partners,
- homosexual orientation, both in men (the incidence of anal cancer is significantly increased) and in women.
With immunosuppression and diabetes mellitus, papillomas, as a rule, are multiple and merge with each other. With genital papillomavirus infection in a pregnant woman, there is a high risk of infection of the baby in utero or during childbirth. At the same time, human papillomavirus infection (HPV types 6, 11 and 16, 18) can persist for a number of years in the cells of the mucous membrane of the child’s mouth and cause juvenile laryngeal papillomatosis. Juvenile laryngeal papillomatosis can develop if the mother has a history of genital warts, as well as with a subclinical course of her genital HPV infection. Children can be carriers of mucocutaneous types of the virus even if they are not present in the mother’s genital tract at the time of birth.
In this regard, one should remember about the increased detection of the virus in the woman’s reproductive tract during pregnancy (thrush of pregnant women), when the fetus becomes infected.
Cases of papillomatosis of the larynx, trachea, and bronchi in children born by cesarean section have been described, indicating the possibility of transplacental transmission of infection. This indicates the inappropriateness of delivery by cesarean section, the only purpose of which is to prevent infection of the newborn with the virus. Extrasexual transmission of genital warts is also possible
- when bathing children in a shared bath with adults infected with the virus,
- when using towels infected by adults,
- with sexual transmission of HPV infection to children.
Thus, unlike adults, infection of children with anogenital warts can occur in different ways.
Clinical manifestation of genital infection is accompanied by the appearance of genital warts (condylomas). The absence of clinical and histological signs when detecting human papillomavirus DNA indicates a latent (asymptomatic) infection.
Vaccines
There are currently two vaccines that protect against human papillomavirus types 16 and 18, which cause at least 70% of cervical cancers. These vaccines may also provide some cross-protection against other, less common HPV types that cause CC. One of these vaccines also protects against HPV types 6 and 11, which cause anogenital warts.
Currently, 2 vaccines against human papillomavirus infection are registered in the Russian Federation in accordance with the established procedure: the Gardasil vaccine and the Cervarix vaccine. The development and registration of vaccines against human papillomavirus infection in our country have determined the possibility of primary prevention of cervical cancer.
More about vaccines
High oncogenic HPV type
The above-described viruses of types 16 and 18 are at high risk of cancerous degeneration of the epithelium.
Also included in this type are strains 70, 68, 64, 59, 50, 39, 33, 31.
The second group is of average oncogenic risk.
It is possessed by strains type 58, 56, 53, 52, 45, 35, 30.
Strains 73, 72, 61, 51, 44 to 40, 34, 32, 13, 11, 6, 3 are considered low risk.
Low-risk viruses often cause only the formation of benign papillomas or condylomas.
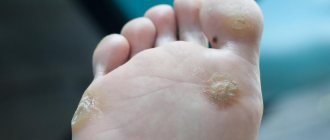
Such formations in men more often affect the skin of the penis (leaves of the foreskin, coronary groove, less often found inside the urethra on the mucous membrane).
In women, the location of these growths is the labia minora and majora, and the perianal region.
Risk areas include skin or mucous membranes injured during sexual intercourse and areas of epithelial maceration.
Latest epidemics
Cervical cancer is the second most common cancer among women, with an estimated 530,000 new cases occurring in 2012.
Every year, about 14,000 new cases of cervical cancer are registered in Russia, which accounts for more than 30% of all malignant neoplasms of the female genital organs. The incidence rate continues to increase. More than 160,000 women are registered for this pathology in oncological institutions in the country. The average probability of developing cervical cancer for every woman in Russia during her lifetime is 0.53%.