Syphilis: symptoms and first signs, how to treat syphilis
Symptoms of syphilis depend on the stage of the disease, age and gender of the patient. The course of this venereal chronic disease may have its own characteristics in each specific case. It is even capable of being asymptomatic for the time being in a latent state.
A distinctive feature of treponema pallidum is its exceptional contagiousness, which is why it is so important to survey the population in order to avoid an epidemic of this disease.
The worst thing is when it has a hidden course and the person does not even realize that he is a carrier of syphilis and poses a danger to his family and others.
How is it transmitted?
Syphilis is caused by Treponema pallidum, which lives in the external environment for only 3 minutes. Therefore, the main route of transmission of the disease is sexual. Infection of the fetus is possible in utero (vertical route) or intrapartum, when the child passes through the mother’s birth canal.
The household route of transmission is uncommon; infection is possible from persons with the tertiary stage of syphilis, when treponema pallidum gets on dishes, linen, towels, etc. from decaying gums. Hematogenous transmission of syphilis through blood transfusion cannot be ruled out.
Cases of infection of medical workers through contact with the blood of a patient are not that rare. It is possible to become infected through “bloody” objects: a shared toothbrush, razor, manicure set, etc.
Syphilis - incubation period
The incubation period is a period of illness that lasts from the moment Treponema pallidum enters the body until the appearance of the first signs of syphilis (see photo), including chancre in combination with regional lymphadenitis. During this period, there is a gradual increase in the number of pathogen cells at the site of their introduction into the patient’s body. Treponema reproduces by division on average once every 30-32 hours.
This period of the disease is characterized by the absence of registered clinical and serological changes in the patient’s body; it lasts on average 3-4 weeks, it can be shortened to 8-15 days or lengthened to 108-190 days. A shortening of the incubation period occurs, as a rule, when the body is simultaneously infected from 2 sources; it is lengthened when taking antibiotics after the moment of infection, for example, for a sore throat, although it should be noted that an increase in the incubation period is not always due to the use of antibiotics.
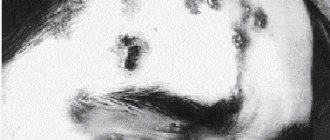
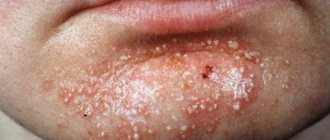
The difference between acne due to syphilis and chickenpox
Smallpox syphilide is most easily confused with chickenpox.
This disease is diagnosed mainly in childhood.
In adults it is more severe.
The difference is a pronounced intoxication syndrome.
It occurs 2-3 days before acne appears.
Severe hyperthermia, cephalalgia, myasthenia gravis, and sore throat are noted.
There are many foci of rashes, and they are located in groups.
While with syphilis there are few of them, and they are single.
Another feature of chickenpox is the extremely rapid transformation of morphological elements.
The entire cycle can take only 8 hours.
First, pink spots form.
From them papules are formed.
They turn into bubbles.
They usually contain completely clear liquid.
Unlike syphilis, in which the contents of the vesicles are often purulent.
With chickenpox, there is severe itching of the skin.
Primary syphilis
After the end of the incubation period, the characteristic first symptoms of syphilis appear. At the site of penetration of the treponemas, a hard chancre is formed, a specific round erosion or ulcer, with a hard, smooth bottom and “turned-up” edges. The size of the formations can vary from a couple of mm to several centimeters. Hard chancre can disappear without treatment. Erosions heal without a trace, ulcers leave flat scars.
The disappearance of chancre does not mean the end of the disease: primary syphilis only passes into a latent form, during which the patient is still infectious to sexual partners.
After the formation of hard chancre, local enlargement of the lymph nodes begins after 1-2 weeks. When palpated, they are dense, painless, and mobile; one is always larger than the others. After another 2 weeks, the serum (serological) reaction to syphilis becomes positive, from this moment primary syphilis passes from the seronegative stage to the seropositive stage. The end of the primary period: body temperature may rise to 37.8 - 380, sleep disturbances, muscle and headaches, and joint aches appear. Dense swelling of the labia (in women), the head of the penis and the scrotum in men is possible.
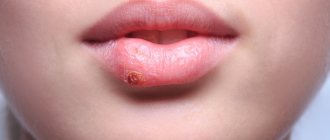
Chancre
It is formed, as a rule, at the site of penetration of Treponema pallidum (with genital contact - in the genital area, with oral-genital contact - in the oral cavity, in the lip area, etc.).
The formation of chancre occurs in several stages:
- formation of a small spot, pink-red color;
- formation of an erosive defect;
- compaction of the erosion bottom, color change to bright red. The erosion is covered with a transparent or brown film.
With timely treatment or, on the contrary, transition to the next stage of syphilis, the chancre again enters the spot stage and then completely disappears. As a rule, such a tumor does not cause discomfort in an infected person. Slight itching may occur in the area of erosion.
You might be interested! Streptoderma in a child: how does it start and how to treat it?
Chancre is classified according to the following criteria:
- by quantity (single, multiple);
- according to the depth of the skin lesion (erosive - affects only the superficial layers, ulcerative - the lesion affects the deep layers of the skin);
- by size (dwarf - less than 10 mm, medium - 10-20 mm, giant - more than 40 mm).
There are also atypical forms of chancre, which are extremely rare.
These include:
- chancre-amygdalid : a hard chancre located on the tonsil (in the ulcerative form of this process, a single tonsil is affected, it becomes compacted and a bright red ulceration with smooth edges is formed on the surface; in the angina-like form, a tissue defect does not form, the tonsil is dense, painless, pale treponema are found on its surface);
- chancre-felon (the clinical picture is similar to streptococcal felon, however, with a syphilitic nature, acute inflammation does not develop);
- indurative edema manifests itself in the genital area in the form of sharp swelling and changes in tissue turgor.
As a rule, diagnosing a typical chancre does not cause much difficulty. Its distinctive feature is the enlargement of regional lymph nodes, which remain dense and painless throughout the course of the primary stage.
Complications of chancroid:
- balanitis;
- balanoposthitis;
- phimosis;
- paraphimosis;
- phagedenism;
- gangrene.
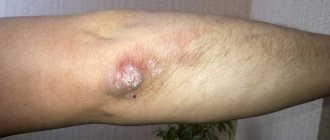
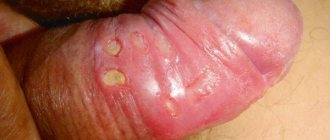
Photo
The photograph shows the typical shape of chancre. There is a clear demarcation of this formation from healthy skin, a hyperemic surface of erosion, covered with a thin transparent film.
Secondary syphilis
The infection generalizes by 3 months from the moment of infection and lasts 3-5 years, this period is characterized by multiple different-looking rashes in various organs and tissues, and therefore absolutely any symptoms depending on which system/organ is affected more and how much it is affected was previously compromised, that is, was he healthy at the time of the defeat - if so, then the manifestations of syphilis will be minimal.
During this period, there are prodromal symptoms (as with colds - general malaise, pain in muscles, joints, the appearance of fever), they last 7-10 days until the appearance of syphilomas (roseolous-papular rashes) - often these are small red spots with clear boundaries , not merging with each other. When pressed, they disappear, and then appear, or may turn yellow due to the destruction of red blood cells. These rashes do not destroy tissue and, with antisyphilitic treatment, disappear instantly. These rashes are recurrent in nature, that is, they appear again, but are not as pronounced and in much smaller quantities.
Publications in the media
Syphilis is an infectious disease caused by Treponema pallidum, transmitted primarily through sexual contact, with a chronic relapsing course and a characteristic periodicity of clinical symptoms, which can affect all organs and systems. Frequency . In Russia in 2001, the incidence was 143.6 per 100,000 population.
Classification • Primary syphilis •• Seronegative •• Seropositive • Secondary syphilis •• Fresh •• Recurrent •• Latent • Tertiary syphilis •• Active •• Latent • Latent syphilis •• Seropositive early •• Seropositive late • Congenital early syphilis •• Late • • Latent • Neurosyphilis • Visceral syphilis.
Etiology. The causative agent is pale treponema (Treponema pallidum), spiral-shaped, 4-14 microns long and 0.2-0.25 microns in diameter, has 8-12 uniform curls, can exist in three forms - spiral, cystic and L-form. The most common (classical) course of syphilis is due to the presence of a spiral form of the pathogen; other forms probably maintain a long latent course.
Epidemiology. The source of infection is a sick person. Conditions of infection: the presence in the material from the patient of a sufficient number of virulent Treponema pallidum and violation of the integrity of the skin and mucous membrane. The main route of infection is direct contact (usually sexual) with a sick person. With congenital syphilis, infection occurs in utero - through the vessels of the placenta. Treponema pallidums that have entered the body spread through the lymphatic system, actively multiply and enter various organs and tissues, which causes certain manifestations of the disease. Over time, the number of Treponema pallidum in the patient’s body decreases, but the tissue reaction to the pathogen becomes more violent. They admit the possibility of a long (many years) asymptomatic course of syphilis from the very beginning of the disease with the subsequent development of damage to the nervous system and visceral forms of the disease.
CLINICAL PICTURE. In untreated patients, acquired syphilis lasts for many years. In the classical course of the disease, there are 4 periods: incubation, primary, secondary, tertiary.
The incubation period lasts from the moment of infection until the appearance of the first clinical symptom - chancre (on average - 20-40 days). Sometimes it is reduced to 10–15 days with massive infection, which is accompanied by multiple or bipolar chancre, as well as with superinfection. An extension of the incubation period to 3–5 months is often observed with severe concomitant diseases or after treatment with low doses of antibiotics.
Primary period
• Continues from the moment of appearance of chancroid until the appearance of generalized rashes (6–7 weeks). It is characterized by the development at the site of penetration of pale treponema (usually in the genital area), chancre (ulсus durum, primary syphiloma) and regional lymphadenitis.
• Clinical signs of chancre •• Erosion (or ulcer) with the absence of acute inflammatory phenomena •• Regular round or oval outline, clear boundaries •• Size of a small coin •• Raised above the surrounding healthy skin (mucous membrane) •• Smooth, shiny, bluish-red bottom, flat (saucer-shaped) edges •• Scanty serous discharge •• Densely elastic (cartilaginous) infiltrate at the base, painlessness •• Chancre is often single, multiple chancre is rarely observed (in about 20% of patients) •• Atypical hard ones are also isolated chancre: indurative edema (painless dense swelling of the foreskin or labia), chancre-amygdalitis (dense swelling of the tonsil) and chancre-felon (simulates ordinary felon).
• Chancre can be complicated by a secondary infection: acute inflammatory reactions in the circumference of the chancre (if localized in the genital area - vulvitis or balanoposthitis, often leading to phimosis or paraphimosis). When complicated by fusospirillosis symbiosis, necrosis of the bottom and edges (gangrenization) of chancre occurs. Repeated gangrenization (phagedenism), usually observed in persons suffering from alcoholism, leads to significant tissue damage.
• Regional lymphadenitis (accompanying bubo, regional scleradenitis) is the second obligatory symptom of primary syphilis, occurs 7–10 days after the appearance of chancre •• Enlargement and hardening of the lymph nodes closest to the chancre •• When chancre is localized on the genitals, the inguinal lymphatics undergo changes nodes: they are enlarged to the size of a bean, sometimes larger, dense, not fused to each other and to the surrounding tissues, mobile, painless on palpation, the skin over them is not changed •• Characterized by enlargement of several lymph nodes. Scleradenitis can be bilateral or unilateral. Sometimes a strand of regional lymphangitis can be seen and palpated between the chancre and enlarged lymph nodes. •• At the end of the primary period, specific polyadenitis develops (moderate enlargement of all groups of lymph nodes), sometimes low-grade body temperature and general weakness are noted.
Secondary period
• Characterized by generalization of infection and lasts 3–4 years.
• All organs and systems can be affected, but the main manifestations are rashes on the skin and mucous membranes (secondary syphilides). The rashes of each of the attacks of the secondary period, having existed for about 1.5–2 months, undergo spontaneous regression, and after a more or less long latent period they appear again.
• The first rash, which marks the beginning of the secondary period, is particularly bright and abundant in the rash (secondary fresh syphilis). It is usually accompanied by fading chancroid and pronounced polyadenitis.
• Repeated episodes of rashes (secondary recurrent syphilis) alternate with periods of complete absence of manifestations (secondary latent syphilis). The rash with secondary recurrent syphilis is less abundant and tends to cluster. In the first half of the year, the rashes are accompanied by gradually fading polyadenitis.
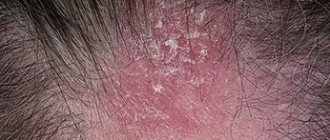
• Secondary syphilides have a number of common features that distinguish them from other skin rashes: they are ubiquitous, have a benign course, there are no febrile symptoms, there are also no acute inflammatory phenomena and subjective sensations, they are resistant to local treatment, and quickly disappear under the influence of therapy. In the secondary period, 5 groups of syphilides are distinguished •• Syphilitic roseola (observed in 75–80% of patients): a pink spot 0.5–1 cm in size, irregularly rounded in outline, does not peel off, disappears with pressure •• Syphilitic papule (observed just as often , like roseola): a bluish-red nodule of dense consistency with peeling along the periphery (Biette's collar). Varieties of syphilitic papules ••• Lenticular (lenticular): size 0.3–0.5 cm ••• Miliary: the size of a poppy seed ••• Nummular (coin-shaped): the size of a large coin, tendency to cluster ••• Seborrheic: localized on the face, forehead skin and is distinguished by oily scales on the surface ••• Erosive (weeping): characterized by an erosive or weeping surface, localized on the mucous membrane or in the folds of the skin ••• Condylomas lata (vegetative papules) are located in places of skin friction (inguinal region), are distinguished by their large size, vegetation, erosive surface ••• Horny papules of the palms and soles are characterized by a powerful development of the stratum corneum on the surface, very reminiscent of calluses ••• Psoriasiform papules: pronounced peeling on the surface •• Syphilitic pustule (rarely observed): noted in weakened patients with a severe (malignant) course of the process. Clinical varieties: acne, smallpox, impetiginous, syphilitic ecthyma, syphilitic rupee •• Syphilitic baldness - rapidly developing small-focal or diffuse hair loss on the head without inflammatory changes in the skin, usually observed in the second half of the disease •• Syphilitic leukoderma (syphilide pigmentosa), more often noted in women, it is localized on the lateral and back surfaces of the neck (necklace of Venus), often on the skin of the torso; On the affected areas, against the background of hyperpigmentation, hypopigmented round spots 0.5–1 cm in size appear.
• The mucous membrane of the pharynx is often affected, where syphilitic tonsillitis occurs (erythematous, papular and pustular-ulcerative), differing from ordinary tonsillitis by sharp boundaries, the absence of acute inflammatory reactions, fever and pain. With rashes on the vocal cords, hoarseness of the voice is noted.
• With secondary syphilis, damage to internal organs, the central nervous system, bones, joints, organs of vision, hearing, etc. is possible. •• Bone damage is noted in 5% of patients in the form of diffuse periostitis with painful swelling, night pain in the bones; osteoperiostitis is observed less frequently. The bones of the skull and tibia are most often affected •• Joint damage usually occurs as a polyarthritic synovitis with the formation of effusion in the joint cavity •• The most important specific lesions of the internal organs of the secondary period include syphilitic hepatitis (enlarged and painful liver, increased body temperature, jaundice) , gastritis, nephrosonephritis, myocarditis •• Damage to the central nervous system in the secondary period is called early neurosyphilis. Damage to the meninges and blood vessels is typical. During a neurological examination, as well as during the analysis of cerebrospinal fluid, syphilitic meningitis (often asymptomatic), syphilis of the brain vessels (meningovascular syphilis), rarely - syphilitic neuritis and polyneuritis, neuralgia are diagnosed.
Tertiary period
• Develops in approximately 40% of patients in the 3rd–4th year of the disease and continues indefinitely. The transition of the disease to the tertiary period is facilitated by inadequate treatment or its absence, severe concomitant diseases, alcoholism, etc.
• Distinctive features of the tertiary period are the appearance of false inflammatory infiltrates in the form of tubercles and gummas, prone to decay, followed by extensive destructive changes in the affected organs and tissues; productive nature of inflammation with the formation of infectious granuloma; a small number of rashes (the number of tubercles is in the tens, gumma - in units); ubiquity of lesions, undulating course.
• In case of clinical manifestations, tertiary active syphilis is diagnosed; in the absence of such, tertiary latent syphilis is diagnosed.
• Relapses of tertiary lesions are observed infrequently, they are separated from each other by a long (sometimes many years) latent period. The lifespan of tertiary syphilides is calculated in months or years; they are characterized by low infectivity due to the small number of pale treponema in the tissues. Classic serological reactions are negative in 30% of patients with tertiary syphilis. The skin, mucous membrane and skeletal system are most often affected. Skin lesions are represented by tubercular and gummous syphilides.
• Tuberous syphilide is a small dense tubercle located in the thickness of the skin, hemispherical in shape the size of a cherry pit, bluish-red in color. After a few weeks or months, the tubercle softens and ulcerates to form a round, rather deep ulcer, with smooth, steep, dense edges. Gradually, the ulcer epithelializes and turns into an atrophic scar pigmented along the periphery, on which new rashes never appear.
• Gummous syphilide (gumma) is a node of dense consistency the size of a walnut, rising above the skin level, painless on palpation, not fused with the surrounding tissues. The skin over it is initially unchanged, then becomes bluish-red. Subsequently, the gummous node softens in the center and is opened with the release of a glue-like exudate. The resulting defect quickly increases in size and turns into an ulcer. It is painless, clearly demarcated from the surrounding skin by a ridge of dense, undisintegrated gummous infiltrate, its edges are steep, the bottom is covered with necrotic masses. A gummous ulcer lasts for months, and with secondary infection - even years. After the gumma heals, a characteristic star-shaped scar remains. In some cases, the contents of the gum are replaced by fibrous tissue with the formation of dense nodes. Gummas of the mucous membranes are often noted. Most often the membrane of the nasal cavity is affected, then the pharynx. Gummous lesions of the tongue, hard and soft palate, nose, pharynx, larynx lead to severe, often irreparable disturbances in speech, swallowing, breathing, and change the appearance of the patient (saddle nose, complete destruction of the nose, perforation of the hard palate). Among gummous lesions of other organs, syphilides of the periosteum, bones and joints are most often observed; The bones of the legs, forearms, skull, knee, elbow and ankle joints are affected.
Congenital syphilis is transmitted to the fetus of a sick mother through the placenta, mainly in the first 3 years after the mother is infected.
• Pregnancy outcomes with syphilis: late miscarriages, premature births, full-term births. Stillbirths are frequently reported. Children are born with active manifestations or latent syphilis.
• Depending on the duration of the syphilitic infection, periods of congenital syphilis are distinguished: fetal syphilis, early congenital syphilis (infant syphilis and early childhood syphilis are distinguished), late congenital syphilis (after 4 years) •• Fetal syphilis (fetal damage by syphilis occurs at fifth month of pregnancy) is accompanied by changes in internal organs, and somewhat later in the skeletal system. Specific lesions of the internal organs of the fetus are manifested by intercellular infiltration and proliferation of connective tissue. Widespread and severe lesions of the internal organs of the fetus often lead to late miscarriages and stillbirths •• Early congenital syphilis can first appear both in infancy (up to 12 months) and in early childhood (1–4 years) ••• Syphilis in infants most often manifests itself in the first 3 months of life and is very unique. In children born from untreated mothers with active manifestations of secondary syphilis, congenital syphilis is an extremely severe disease affecting almost all internal organs, the central nervous system and specific changes in the skin and mucous membranes ••• An early manifestation of syphilis in this period is syphilitic pemphigus. The rashes are localized mainly on the skin of the palms and soles, less often on other areas of the skin. Bubbles the size of a pea and a cherry are initially serous, then purulent, sometimes hemorrhagic, located on an infiltrated base and surrounded by a zone of specific papular infiltrate of a bluish-red color ••• Diffuse Hochsinger infiltration is usually localized on the soles, palms, face and scalp. The lesion is clearly demarcated, with a smooth shiny surface of bluish-red color; is distinguished by a densely elastic consistency, leading to the formation of cracks that have radial directions in the circumference of the mouth and leave lifelong radiant Robinson-Fournier scars ••• Widespread or limited roseolous, papular and pustular rashes in all their varieties, similar to those in the secondary period of syphilis, are also observed. Skin rashes are often preceded by an increase in body temperature ••• Damage to the mucous membranes often occurs in the form of a syphilitic runny nose: specific erosive-papular hyperplastic anterior rhinitis. Breathing through the nose becomes extremely difficult, which makes the act of sucking impossible. As a result of ulceration of the papular infiltrate of the nasal septum, its destruction with deformation of the nose is possible ••• Lesions of the skeletal system: lack of active movements in the limbs and pain in passive movements, caused by the formation of gummas in the epimetaphyses of long tubular bones with a tendency to fractures (Parro’s pseudoparalysis, Wegner’s disease) • •• Specific lesions of internal organs often begin in utero; their diffuse nature causes severe congenital syphilis and significant mortality in the first weeks and months of a child’s life. Liver damage is detected in the form of its enlargement and thickening. Rarely, jaundice is noted with atrophic cirrhosis of the liver. Damage to the spleen is often observed. Specific lung damage in the form of white pneumonia is rarely recorded; often occurs as a complication of pneumonia of various etiologies. Kidney damage (glomerulonephritis, nephritis, nephrosonephritis) is noted in 14% of patients. The cardiovascular system is affected early, but rarely (myocarditis, endocarditis, pericarditis) ••• One of the most common lesions of the central nervous system is specific meningitis with convulsions, paralysis and anisocoria. Increased cytosis, an increase in the amount of protein, and positive globulin reactions are noted in the cerebrospinal fluid. Some children develop hydrocele at 2–3 months of age. Among the sense organs in infants, the eyes are affected. Already at the birth of a child, it is possible to detect changes in the retina and macular membrane (chorioretinitis), damage to the optic nerve ••• Limited large-papular (usually weeping) rashes such as condylomas lata are often observed on the skin, erosive papules are often observed on the mucous membranes; bones are often affected (syphilitic periostitis of long tubular bones) •• Late congenital syphilis appears at the age of 5–17 years and resembles the tertiary period of syphilis in its clinical manifestations. Signs of late congenital syphilis are divided depending on the degree of specificity into absolute, or unconditional; relative, or probable (observed more often with late congenital syphilis, but also noted with other diseases); dystrophies (can be a consequence of both congenital syphilis and other diseases) ••• Absolute signs include Hutchinson’s triad: Hutchinson’s teeth (barrel-shaped or chisel-shaped incisors, hypoplasia of the chewing surface with a semilunar notch along the free edge), parenchymal keratitis (uniform milky white clouding of the cornea with photophobia, lacrimation and blepharospasm), labyrinthine deafness (inflammatory phenomena and hemorrhages in the inner ear in combination with dystrophy of the auditory nerve) ••• Relative signs are assessed in conjunction with other manifestations. These include: syphilitic chorioretinitis (characteristic of the “salt and pepper” pattern on the fundus), saber-shaped shins (the result of diffuse osteoperiostitis with reactive osteosclerosis and anterior curvature of the bones of the legs), Robinson-Fournier scars (in the circumference of the mouth after Hochsinger infiltrations), syphilitic gonitis , occurring as chronic allergic synovitis (distinguished by the absence of sharp pain, fever and dysfunction of the joint), buttock-shaped skull (sharply protruding frontal tubercles with a groove located between them), nasal deformities (saddle-shaped, lorgnette-shaped, etc.), dental dystrophy (tooth Muna - underdevelopment of the chewing tubercles of the first molars, Fournier's pike tooth - a change in the canine with thinning of its free end) ••• Dystrophies with congenital syphilis: Ausitidian sign (thickening of the sternal end of the clavicle), Olympic forehead (increase in the frontal and parietal tubercles), high (Gothic ) palate, infantile (shortened) little finger of Dubois-Hissar, absence of the xiphoid process of the sternum, widely spaced upper incisors, etc. Only the presence of several dystrophies in combination with other signs of syphilis and anamnesis data can, in unclear cases, help make a diagnosis of congenital syphilis.
Research methods • In the primary period: detection of pale treponema in the discharge from chancre • Serological reactions •• RSC (type of von Wasserman reaction) with cardiolipin and treponemal Ag and microprecipitation reaction with cardiolipin Ag (VDRL - with inactivated blood serum, RPR - with plasma blood, UJR - with active blood serum; ART - automated reagin test, etc.). Positive results are expressed by pluses (from + to ++++). In case of a sharply positive reaction, a study is carried out with various dilutions of serum (from 1:10 to 1:320). Reactions are positive from the middle of the primary period and during the secondary period; in the tertiary period they can be negative in 50% of patients •• Treponema pallidum immobilization test: carried out for false-positive serological reactions, assessed as negative when less than 20% of Treponema pallidum are immobilized, weakly positive - 21– 50%, positive - over 50% •• RIF: becomes positive in the majority of patients with syphilis already in the primary seronegative period; the results are assessed as positive (from + to ++++); positive in all periods of syphilis (including late forms) in almost all patients •• ELISA •• Passive hemagglutination test
TREATMENT • Specific treatment is prescribed after clinical and laboratory confirmation of the diagnosis (exception: preventive treatment of persons who have had sexual and close household contact with patients with early forms of syphilis, if no more than 2 months have passed since the contact) • Preventive treatment is carried out for women who received treatment before pregnancy , in whom by the beginning of pregnancy there was no complete negativity of the CSR (a complex of serological reactions, including various methods for detecting antibodies to the pathogen, for example, the von Wasserman reaction, microprecipitation reactions, less often others), as well as all women who began treatment during pregnancy, regardless of its term. And also to children born without manifestations of syphilis from an untreated mother; with late specific treatment for the mother (from 32 weeks of pregnancy); in the absence of negativity of CSR at the time of birth or seroresistance in the mother.
Drug therapy • Causal therapy: benzylpenicillin preparations are the mainstay in the treatment of all forms of syphilis. In case of intolerance: penicillin drugs, alternative drugs specified in the guidelines are prescribed (erythromycin, tetracycline, oleandomycin + tetracycline, doxycycline, cefazolin, etc.).
Treatment of primary syphilis: method No. 1 - two injections of benzathine benzylpenicillin at a dose of 2.4 million units with an interval of 7 days, or three injections of benzathine benzylpenicillin at a dose of 2.4 million units once every 5 days; Method No. 2 - benzathine benzylpenicillin + benzylpenicillin procaine + benzylpenicillin at a dose of 1.8 million units 2 times a week, a total of 5 injections, or benzathine benzylpenicillin + benzylpenicillin procaine at a dose of 1.5 million units 2 times a week, a total of 5 injections; Method No. 3 - penicillin procaine at a dose of 1.2 million units daily for 10 days or 600,000 units 2 times a day for 10 days; Method No. 4 - water-soluble penicillin intramuscularly every 6 hours for 10 days.
Treatment of secondary and early latent syphilis: method No. 1 - three injections of benzathine benzylpenicillin at a dose of 2.4 million units with an interval of 7 days, or six injections of benzathine benzylpenicillin at a dose of 2.4 million units once every 5 days; Method No. 2 - benzathine benzylpenicillin + benzylpenicillin procaine + benzylpenicillin at a dose of 1.8 million units 2 times a week, a total of 10 injections, or benzathine benzylpenicillin + benzylpenicillin procaine at a dose of 1.5 million units 2 times a week, a total of 10 injections; Method No. 3 - penicillin procaine at a dose of 1.2 million units daily for 20 days or 600,000 units 2 times a day for 20 days; Method No. 4 - water-soluble penicillin intramuscularly every 6 hours for 20 days.
Treatment of other forms of syphilis - see Methodological recommendations “Treatment and prevention of syphilis”, approved by the Ministry of Health of the Russian Federation (1999).
Contraindications. Tetracyclines - during pregnancy and children under 8 years of age.
Clinical and serological control after the end of treatment • After preventive treatment, once 3 months after treatment • For primary seronegative syphilis - 3 months • Patients with early forms of syphilis who had positive DSR results before treatment are subject to clinical and serological control until the DSR is completely negative and then another 6 months • For late forms, latent, visceral and neurosyphilis - 3 years.
Prevention • Public: free treatment, active detection, examination and involvement of contact persons in treatment, screening for syphilis of donors, pregnant women, all inpatients, workers of food enterprises and child care institutions • Individual: use of condoms.
ICD-10 • A50 Congenital syphilis • A51 Early syphilis • A52 Late syphilis • A53 Other and unspecified forms of syphilis
Tertiary syphilis
Tertiary syphilis is characterized by a long latent course. It can appear after 3-4 years (with complete absence of treatment, or with insufficient treatment). Most often, this form of pathology can be found in patients suffering from chronic alcoholism, tuberculosis or other infections.
During this period, a small amount of dense infiltrates, localized in the subcutaneous tissue or in deeper tissues, is found on the patient’s skin and mucous membranes. After some time, they disintegrate, and in their place painless ulcers appear, which scar only after a few months or years. It should be noted that such syphilides are not accompanied by subjective disorders and do not disturb the general condition of the patient. They contain very little pathogen, and therefore are practically non-contagious.
Rubbers and gums: flow features
The rubber layer in the bones eats away, which leads to fractures. The affected liver increases in size, which simulates various hypertrophies, subsequent scarring leads to cirrhosis. On the skin, gummas appear as subcutaneous nodes, which eventually open, forming an ulcer. The ulcers, decomposing, increase in size, then, over time, clean off and heal, leaving a scar. Rarely, gummous nodes are not opened; in such cases, they can resolve without leaving scars on the skin. Without proper treatment, gummas can affect tissue for years, penetrating deeper, involving muscles, periosteum, bones and joints. If the mucous membrane of the nose or palate is affected, gummas can deform them to the point of impaired breathing and disfigurement of the nose. Gummous formations usually affect the nasal septum, which stimulates the secretion of mucous masses. As a result, a dry crust forms, but if it is peeled off, there will be bleeding. Changing the shape of the nose occurs when the nasal bones are rejected. The soft palate becomes deformed and collapses due to the same processes. Damage to the aorta leads to an aneurysm, which can lead to atrophy. Pressure from the sternum and adjacent parts of the ribs on the aorta often provokes hemorrhage, leading to death. Damage to organs at this stage of syphilis leads to various types of disorders, often incompatible with life.
Congenital syphilis
It is transmitted from a sick mother when treponemes penetrate the placenta into the fetus. Syphilis infection can occur both during conception and much later. Regardless of the time of infection, pathological tissue changes are observed only in the VI-VII months of pregnancy, so active prevention of syphilis in the early stages will help give birth to a healthy child.
The possibility of transmitting pathogens through the father's sperm has not yet been proven, so all preventive measures usually concern the expectant mother. These include: identification of sick women in the early stages, full registration of pregnant women, monitoring the treatment of infected persons. In order to prevent the development of negative changes, mandatory regular examinations of pregnant women are carried out for the presence of treponemas and external signs of congenital syphilis.
Features of syphilis symptoms in men and women
The secondary and tertiary periods have almost the same symptoms. Differences in symptoms for men and women are present only in the primary period, when chancre appears on the genitals:
- gangrenous chancre on the penis - there is a possibility of self-amputation of the distal part of the penis;
- chancre on the cervix. Signs of syphilis, when hard chancre is located on the uterus in women, are practically absent and can only be detected during a gynecological examination;
- chancre in the urethra is the first sign of syphilis in males, which is manifested by discharge from the urethra, a dense penis and an inguinal bubo.
Classification of the disease
Syphilis is divided into forms and types, due to different timing, routes of spread and varied symptoms.
According to the degree of damage, syphilis is divided into:
- primary;
- secondary;
- tertiary.
In addition, it can be:
- hidden,
- congenital,
- late,
- chronic.
Primary syphilis - stage 1 of infection, a distinctive feature is the appearance of chancre. Chancres often appear on the genitals, since the sexual tract is the most common route of transmission of infection. Chancres can also appear on the face, mouth, mammary glands, and legs. Primary syphilis has no other manifestations.
Secondary syphilis - stage 2 of infection. It is characterized by the appearance of a papular rash. At this time, the patient experiences inflammation of the lymph nodes, damage to the nervous and musculoskeletal systems.
Tertiary syphilis develops in people who have not received treatment or have not completed treatment for the disease. Syphilitic granulomas appear on the mucous membrane, skin, bones, and internal organs, which destroy these structures. Currently, this stage is rare, since at stages 1 and 2 the disease can be successfully treated.
Latent syphilis is considered the most dangerous because the patient has no symptoms, but it poses a danger to others. Syphilis is classified as late if more than 2 years have passed since infection and symptoms have just appeared. Syphilis, which has developed over decades, is called chronic; it slowly destroys the body, and is not always accompanied by symptoms.
Diagnostics
Syphilis is diagnosed by examination, characteristic signs and laboratory tests:
- Examination by a dermatovenerologist. He asks the patient in detail about the course of the disease, examines the skin, genitals, and lymph nodes.
- Detection of treponema or its DNA in the contents of gummas, chancre, syphilides using dark-field microscopy, direct immunofluorescence reaction, and PCR.
- Instrumental studies: search for gummas using ultrasound, MRI, CT, X-rays, etc.
- Carrying out various serological tests: Non-treponemal - search for antibodies against treponema membrane lipids and phospholipids of tissues destroyed by the pathogen (Wassermann reaction, VDRL, rapid plasma reagin test). The result obtained may be false positive, i.e. show syphilis where there is none. Treponema - search for antibodies to Treponema pallidum (RIF, RPHA, ELISA, immunoblotting, RIBT).
Remember that for such a serious disease you cannot diagnose yourself “on the Internet” by reading about syphilis and its symptoms. The fact is that the rash and other changes can visually copy those of completely different diseases, so that even doctors are periodically misled.
Consequences of syphilis
If left untreated, syphilis gradually spreads throughout the body and affects more and more healthy tissues and organs. Sometimes there is temporary relief, after which the patient’s condition sharply worsens. Complications of syphilis depend on its stage.
Primary syphilis can be complicated by the following conditions:
- tissue necrosis at the location of the chancre;
- balanitis;
- phimosis;
- paraphimosis
With secondary syphilis, the following complications are noted:
- damage to internal organs by syphilis;
- damage to the nervous system;
- bone damage.
Complications of tertiary syphilis are:
- damage to internal organs;
- brain damage;
- Treponema damage to the tissues of the neck and face;
- pathological fractures of bones when they are affected by syphilis;
- bleeding as a result of vascular rupture.
Acne prognosis for syphilis and complications
Acne with syphilis itself will sooner or later go away on its own.
For some time the disease occurs without symptoms.
But this does not mean that the person is cured.
The rashes often recur.
And in the absence of timely treatment, the disease can progress to the tertiary stage.
She is very heavy.
Accompanied by damage to the central nervous system and internal organs.
Foci of infection can occur in almost any part of the body.
Most often affected:
- bones
- sense organs
- joints
- muscles
Gummas are formed.
Entire sections of tissue die.
They can lead to disability of the patient and often disfigure him.
They often cause organ loss.
For example, the eyes, nose or penis.
In the most unfavorable cases, syphilis ends in death.
How to treat syphilis?
The treatment of syphilis is approached in a comprehensive manner, taking into account many individual factors (age, gender of the patient, stage of development of the disease, the presence of concomitant diseases, general condition of the body, etc.). In addition, all sexual partners of the suspected patient should also be examined for the presence of syphilis and, if necessary, undergo a course of therapy.
If a patient has primary syphilis, then everyone who has had sexual intercourse with him over the past three months must undergo examination and tests. In the case of secondary syphilis - everyone who had contact with the patient over the past year. The timeliness of the therapy itself, as well as the correct selection of modern medications, is important for achieving success in the treatment of this disease.
The most effective method of treating syphilis is the introduction of water-soluble penicillins into the body. This therapy is carried out in a hospital setting for 24 days with injections every 3 hours. The causative agent of syphilis is quite sensitive to penicillin antibiotics, but there is a possibility of an allergic reaction to these drugs or the ineffectiveness of such therapy. In this case, penicillin is replaced with drugs of the tetracycline, macrolide, and fluoroquinolone groups. In addition to antibiotics, natural immune stimulants, vitamins, and immunostimulants are also indicated for syphilis.
Prevention
Standard preventive measures include avoiding casual sex, using condoms, and to prevent occupational syphilis, wearing disposable latex gloves before examination, manipulation and surgery.
Condoms are not 100% protection - the chancre can be located extragenitally (pubis, perineum), and with secondary syphilis, a “necklace of Venus” is formed on the skin. In these cases, the infection from syphilis is transmitted by contact to the partner’s skin.
With syphilis, lifelong immunity is not formed. Having successfully recovered from this disease, you can become infected and get sick again. In this case, the disease will be just as severe. Therefore, there are no vaccinations against syphilis, and there cannot be.
Necklace of Venus (syphilitic leucoderma)
It is a specific sign of syphilis. It forms in the neck area and appears as light, round lesions on the skin that look like a necklace.
Photo
The photograph shows a large number of light spots on the brown surface of the patient's skin, forming a characteristic Venus necklace .
Photo
The photograph shows a patient with a roseola rash , a characteristic manifestation of secondary syphilis.
Forecast
It all depends on the stage of development of the disease and the treatment method. If therapy was started in the early stages of the disease (primary, secondary and early latent syphilis) and is carried out using treponemocidal antibiotics, then in almost all cases without exception, a complete clinical cure occurs, and relapses of early syphilis and the occurrence of late forms of syphilis are prevented.
Treatment of syphilis in pregnant women in the first half of pregnancy in most cases guarantees the birth of a healthy baby. In the case of congenital syphilis, the prognosis is favorable if treatment of the disease was started in a timely manner. Treatment of later forms of the disease is less successful, since it only slows down the progression of the disease, but in all cases it can restore the impaired function of the affected organs and lead to negative serological reactions.